UNIVERSIDAD DE MURCIA
|
|
|
- María Fernández Palma
- hace 8 años
- Vistas:
Transcripción
1 UNIVERSIDAD DE MURCIA DEPARTAMENTO DE MEDICINA INTERNA MEMORIA TESIS DOCTORAL: VALOR PRONOSTICO DE NUEVOS BIOMARCADORES EN INSUFICIENCIA CARDIACA AGUDA SERGIO MANZANO FERNANDEZ MURCIA 2011
2 El contenido de la presente tesis constituye un compendio de trabajos previamente publicados o aceptados para publicación: 1. Complementary prognostic value of Cystatin C, NT-proBNP and cardiac Troponin T in acute heart failure patients. American Journal of Cardiology; 2009 Jun 15; 103 (12): S. Manzano-Fernández, M. Boronat-García, M.D Albaladejo- Otón, Patricia Pastor, Francisco J. Pastor-Pérez, I.P. Garrido, Pedro Martínez- Hernández, M. Valdés-Chavarri, D.A. Pascual-Figal. 2. β-trace Protein and Cystatin C as Predictors of Long Term Outcomes in Patients with Acute Heart Failure. Journal of the American College of Cardiology Sergio Manzano-Fernández, James L. Januzzi, Miguel Boronat-Garcia, Juan Carlos Bonaque-González, Quynh A. Truong, Francisco J. Pastor-Pérez, Carmen Muñoz- Esparza, Patricia Pastor,María D. Albaladejo-Otón, Teresa Casas, Mariano Valdés, and Domingo A. Pascual-Figal. 3. Usefulness of Soluble Concentrations of the Interleukin Family Member ST2 as Predictor of Mortality in Patients with Acutely Decompensated Heart Failure Relative to Left Ventricular Ejection Fraction. American Journal of Cardiology Sergio Manzano-Fernández, MD, Thomas Mueller, MD, Domingo Pascual-Figal, MD, PhD, Quynh A. Truong, MD and James Louis Januzzi, MD.
3 A mi familia y amigos.
4 Índice de Contenidos 1. Complementary prognostic value of Cystatin C, NT-proBNP and cardiac Troponin T in acute heart failure patients. 1.1 Title page Abstract Introduction Methods Results Discussion Tables Table Table Table Table Figures Figure Figure Reference List β-trace Protein and Cystatin C as Predictors of Long Term Outcomes in Patients with Acute Heart Failure. 2.1 Title page Abstract Introduction Methods Results Discussion... 28
5 2.7 Tables Table Table Table Table Table Figures Figures Figure 1A Figure 1B Figure Figures Figure 3A Figure 3B Figures Figure 4A Figure 4B Reference List Usefulness of Soluble Concentrations of the Interleukin Family Member ST2 as Predictor of Mortality in Patients with Acutely Decompensated Heart Failure Relative to Left Ventricular Ejection Fraction. 3.1 Title page Abstract Introduction Methods Results Discussion... 55
6 3.7 Tables Table Table Table Table Tables Table 5A Table 5B Table 5C Figures Figures Figure 1A Figure 1B Figure 1C Figure Reference List Resúmenes en castellano de los artículos 4.1 Artículo Título Objetivo Material y Métodos Resultados Conclusiones Tablas Tabla Tabla Tabla
7 Tabla Figuras Figura Figura Artículo Título Objetivo Material y Métodos Resultados Conclusiones Tablas Tabla Tabla Tabla Tabla Tabla Figuras Figura Figura 1A Figura 1B Figura Figuras Figura 3A Figura 3B Figuras Figura 4A Figura 4B... 97
8 4.3 Artículo Título Objetivo Material y Métodos Resultados Conclusiones Tablas Tabla Tabla Tabla Tabla Tablas Tabla 5A Tabla 5B Tabla 5C Figuras Figuras Figura 1A Figura 1B Figura 1C Figura Apéndice 5.1 Cartas de aceptación de las publicaciones Índice de impacto de las publicaciones
9 Complementary Prognostic Value of Cystatin C, N-terminal pro-b-type Natriuretic Peptide and Cardiac Troponin T in Patients with Acute Heart Failure Sergio Manzano-Fernández, MD 1, Miguel Boronat-Garcia, MD 2, María Dolores Albaladejo-Otón, MD 2, Patricia Pastor, MD 3, Iris Paula Garrido, MD 1, Francisco Jose Pastor-Pérez, MD 1, Pedro Martínez-Hernández, MD 2, Mariano Valdés, Professor 1, Domingo Andres Pascual-Figal, PhD 1 From: 1 Department of Cardiology. Virgen de la Arrixaca University Hospital. Murcia. Spain. 2 Department of Bioquimica. Virgen de la Arrixaca University Hospital. Murcia. Spain. 3 Department of General Surgery. Virgen de la Arrixaca University Hospital. Murcia. Spain. Short title: Cystatin C, NT-proBNP and Troponin T in Acute Heart Failure. Address for correspondence: Sergio Manzano Fernández. Department of Cardiology. Virgen de la Arrixaca University Hospital. Murcia. Spain. Paseo Ramón Gaya. nº 4. 5ºB. CP Murcia. Spain. Tel: ; sergiosmf13@hotmail.com
10 1.2 Abstract We sought to compare the prognostic value of cystatin C over creatinine and Modified of Diet and Renal Disease (MDRD) equation, and to evaluate whether it provides complementary information to cardiac biomarkers in the risk stratification of an unselected cohort of patients with acute heart failure (AHF). We prospectively studied consecutive hospitalized patients with an established AHF diagnosis. Blood samples were collected on hospital arrival to determine cystatin C, ctnt and NT-proBNP. Clinical follow-up was obtained and the occurrence of mortality and/or heart failure (HF) readmission was registered. One-hundred thirty-eight patients (74 [67-80] years, 54% male) were studied. During a median follow up of 261 [ ] days, 60 patients (43.5%) presented adverse events. After multivariable adjustment cystatin C, NTproBNP, ctnt, New York Heart Association Functional Classification class III/IV and diabetes mellitus were identified as independent predictors of mortality and/or HF readmission. In contrast to creatinine and MDRD, the highest cystatin C tertile (>1.50 mg/l) was a significant independent risk factor for adverse events (Hazard Ratio (HR) %CI ;p=0.004). A multimarker approach combining ctnt, NT-proBNP and cystatin C improved risk stratification further, showing that patients with two (HR 2.37, 95%CI ) or three (HR 3.64, 95%CI ) elevated biomarkers had a higher risk of adverse events than patients with no elevated biomarkers (p for trend=0.015). In this unselected cohort, cystatin C was a stronger predictor of adverse events than conventional measures of kidney function. In addition, cystatin C offered complementary prognostic information to cardiac biomarkers and could help clinicians to perform a more accurate risk stratification of patients with AHF. Key words: prognosis, cystatin C, heart failure
11 1.3 Introduction Since patients with acute heart failure (AHF) represent a group at high risk for cardiovascular events and death, risk stratification may be particularly useful in this population 1. N-terminal pro-b-type natriuretic peptide (NT-proBNP) and cardiac troponins (ctn) have emerged as consistent prognostic biomarkers in heart failure (HF) 2-7. Several recent multimarker approaches combining NT pro-bnp and ctn, have been reported to improve the risk stratification of patients with AHF 8, 9. Nevertheless, to the best of our knowledge, the prognostic value of the simultaneous assessment of cystatin C, NT-proBNP and ctnt has not been previously evaluated in this important clinical scenario. Moreover, it has not been clarified whether cystatin C is more useful than creatinine and Modified of Diet and Renal Disease equation (MDRD) in the risk stratification of hospitalized patients with AHF. We designed a prospective study to compare the prognostic value of cystatin C over conventional measures of kidney function, and to evaluate whether it provides complementary information to ctnt and NT-proBNP in the risk stratification of an unselected cohort of patients with AHF. 1.4 Methods Between September 2006 and February 2008, we prospectively included a total of 145 consecutive patients admitted with an initial diagnosis of AHF to the Cardiology Department at the Virgen de la Arrixaca University Hospital. Blood samples were collected for all patients on arrival at the emergency department. After hospital admission, an established final diagnosis of AHF was made in 138 of these cases, which represented the population included in this study analysis. The 7 remaining patients had other established diagnoses. AHF diagnosis was established on the basis of current criteria guidelines and defined as the rapid or gradual onset of signs and symptoms of HF, resulting in unplanned hospitalization, and included new onset AHF and acute decompensation of chronic HF 1.
12 The following baseline clinical characteristics were prospectively recorded in detail on admission: age, sex, hypertension, diabetes mellitus, smoking, hypercholesterolemia, anemia, chronic obstructive pulmonary disease, previous HF, previous stroke, New York Heart Association Functional Classification, etiology of cardiomyopathy, heart rhythm, branch block, need for inotropic support and medication at discharge. Hypertension was defined as elevated systolic blood pressure of >140 mm Hg, diastolic blood pressure >90mm Hg, or when patients had taken antihypertensive drugs. Hyperlipidemia was defined as augmented total cholesterol level of >220 mg/dl, triglyceride >150 mg/dl, decreased high-density lipoprotein level of <40 mg/dl, or when patients had taken drugs of antihyperlipidemia. Anemia was defined using the World Health Organization definition (Hb<12.0 g/dl in women and <13.0 g/dl in men) 10. During the entire hospitalization period, clinical management decisions about each patient were decided by the cardiologist responsible, who was unaware of the patient s cystatin C levels. An echocardiogram was also performed on all patients before hospital discharge, using a Sonos 5500 (Philips, Andover, Massachusetts, USA). The left ventricular ejection fraction (LVEF) was measured using the Simpson biplane method. All patients received standard management as recommended by contemporary guidelines 1. Determination of cystatin C was performed using a BN ProSpec analyzer (Dade Behring). The intra-assay coefficient of variation was 2.5% for 0.9 mg/l and 2.3% for 1.8 mg/l. The inter-assay coefficient of variation was 2.0% for 0.9 mg/l and 2.2% for 1.8 mg/l. Kidney function was also assessed through serum creatinine levels and creatinine-based estimating equation. Estimated glomerular filtration rate was calculated using the simplified MDRD (ml/min/1.73 m 2, [plasma creatinine] [age] 0.203) (the correction factor for women was 0.742) 11. NT-proBNP and ctnt levels were measured by electrochemiluminescence immunoassay using a Modular Analytics E170 analyser (Roche Diagnostics GmbH, Mannheim, Germany). The intra-assay coefficient of variation for NT-proBNP was 1.8% for 221 pg/ml and
13 3.1% for pg/ml. Regarding ctnt, the detection limit provided by the supplier was <0.01 ng/ml. The intra-assay coefficient of variation was 1.2% for ng/ml and 0.8% for 3.00 ng/ml. All patients were clinically followed up for at least 6 months (median 261 days [IQR ]) and the occurrence of clinical events was registered. In patients requiring hospitalization, medical records were carefully reviewed to further characterize the cause of hospitalization. The study endpoint was defined as the combination of mortality and/or HF readmission. The study was approved by the Local Ethics Committee, and informed consent was obtained from each patient at inclusion. Continuous variables were tested for a normal distribution by the Kolmogorov- Smirnov test. Normally distributed data are presented as the mean ± standard deviation and non-normally distributed data as the median (IQR, interquartile data). Categorical variables are expressed as percentages. Since age-, sex-, and racespecific normal ranges for serum cystatin C have not been established, we categorized cystatin C into tertile groups. Patients were grouped according to cystatin C tertiles. Differences in baseline characteristics were compared using ANOVA or the Kruskal- Wallis test for continuous variables and the Chi-Square test for categorical variables. We calculated hazard ratios (HR) derived from the Cox regression analysis to identify predictors of mortality and/or HF readmission during follow-up. The independent effect of variables on prognosis was calculated using a Cox multivariable regression analysis, incorporating covariates with p values <0.10 in the univariable analysis. Cystatin C, creatinine, and MDRD were first entered individually in the multivariable model. Subsequently, creatinine and MDRD were adjusted for cystatin C in a separate multivariable analysis. To compare measures of kidney function as predictors of adverse clinical outcomes cystatin C, creatinine and MDRD were divided by tertiles. Creatinine tertiles were gender-specific to ensure an adequate representation of men and women within each. We determined the unadjusted and multivariable-adjusted risk for the 3 rd and 2 nd tertiles compared with the 1 st tertile for each measure of kidney function. To test the hypothesis that simultaneous assessment of cystatin C, ctnt and
14 NT-proBNP would improve risk stratification, patients were categorized on the basis of the number of elevated biomarkers. Cystatin C, ctnt and NT-proBNP were defined as elevated if their levels were above the median (>1.21mg/L for cystatin C, >0.011ng/ml for ctnt and >3.345pg/ml for NT-proBNP). The cumulative incidence of mortality or HF readmission was estimated according to the Kaplan Meier method and the log-rank statistic was used for comparisons. All p values <0.05 were accepted as statistically significant. Statistical analysis was performed using SPSS 15.0 for Windows (SPSS, Inc., Chicago, IL, USA). 1.5 Results A total of 138 patients were included in the study analysis. The median cystatin C concentration was 1.21 [ ] mg/l, median serum creatinine was 1.15 [ ] mg/dl and mean estimated MDRD was 63±25 ml/min per 1.73m 2. The distribution of baseline characteristics and laboratory parameters by cystatin C tertiles are shown in Tables 1 and 2. Patients with higher cystatin C levels were older, had higher prevalence of anemia and needed more frequent in-hospital inotropic support. Serum creatinine, urea nitrogen, uric acid and NT-proBNP were higher among patients with higher cystatin C levels; whereas serum albumin, hemoglobin and MDRD were lower among these patients. Serum cystatin C concentrations were significantly correlated with serum creatinine and estimated glomerular filtration rate [Spearman rank correlation r=0.77 and (p<0.001), respectively]. Over the study period, a total of 60 patients (43.5%) presented adverse clinical events: 27 patients died and 40 patients were readmitted to hospital owing to HF decompensation. In the univariable Cox regression analysis, all measures of kidney function were associated with a higher risk of adverse clinical events (Table 3). After adjusting for other univariable predictors in the multivariable Cox regression models, cystatin C levels (mg/l, HR %CI ; p=0.037) remained as a significant predictor of adverse events, while serum creatinine and MDRD were no longer
15 significant. When cystatin C, creatinine and MDRD were combined in a single adjusted model, cystatin-c was also the only measure of kidney function that remained as an independent predictor of adverse clinical events (mg/dl, HR %CI ; p=0.037). Other independent predictors of mortality and HF readmission were New York Heart Association Functional Classification class III/IV, diabetes mellitus, NTproBNP and ctnt (Table 3). As shown in the Kaplan-Meier survival analysis (Figure 1), cystatin C tertiles were associated with an incremental rate of adverse clinical events. Mortality and/or HF readmission at 1 year was 65.0% for 3 rd cystatin C tertile, 44.1% for 2 nd cystatin C tertile and 30.1% for 1 st cystatin C tertile (log rank test p=0.001). In the univariable Cox regression analysis and after multivariable adjustment, the highest tertile of cystatin C (>1.50 mg/l) was significantly associated with a higher risk of mortality and/or HF readmission (HR %CI ; p=0.004). In contrast, the highest tertile of creatinine and MDRD only achieved significance in the univariable analysis (Table 4). In a multivariable regression analysis incorporating all 3 biomarkers [elevated Cystatin C (>1.21mg/L; HR 1.92, 95%IC ; p=0.017), NT-proBNP (>3.345pg/ml; HR 1.79, 95%IC ; p=0.029) and ctnt (>0.011ng/ml; HR 2.01, 95%IC ; p=0.003)] each was an independent predictor of mortality and/or HF readmission. By categorizing patients on the basis of the number of elevated biomarkers we found that 23% had elevations in none of the biomarkers, 25% had an elevation in one, 28% had elevations in 2, and 24% had elevations in all 3. There was a significant gradual increase in risk of mortality and/or HF readmission as the number of elevated biomarkers increased (25.8%, 37.1%, 43.6% and 66.7% of patients with 0, 1, 2 and 3 elevated biomarkers respectively reached the study end point; p for trend=0.015). Relative risk of mortality and/or HF readmission, according to the number of the elevated study biomarkers are presented in Fig. 2.
16 1.6 Discussion In this study, we noted a striking relationship between a high cystatin C level and the incidence of mortality and/or HF readmission in hospitalized patients with AHF. In this unselected cohort, we also found cystatin C to be a stronger predictor of adverse clinical events than creatinine and MDRD. Importantly, simultaneous assessment of cystatin C, ctnt and NT-proBNP provided complementary prognostic information and could enable clinicians to perform a more accurate risk stratification of this population. In clinical practice, serum creatinine levels and creatinine based estimating equations are routinely used for the evaluation of kidney function. However, recent data has suggested that cystatin C has a stronger prognosis value than creatinine and MDRD in patients with HF. Shlipak et al 12, first reported cystatin C as a better predictor of mortality than creatinine in selected elderly ambulatory patients with chronic HF. Arimoto et al 13 suggested cystatin C may represent a more useful marker for detecting early kidney dysfunction and recommended discrimination between patients with and without cardiac events in a cohort of patients with mild to moderate HF. These authors showed that patients with elevated cystatin C had a higher cardiac event rate than those with normal cystatin C levels even in patients with normal serum creatinine. Our report mainly differs from these studies in its prospective design and targeted focus on hospitalized patients. Furthermore, it includes an unselected cohort of AHF patients who were treated more according to contemporary recommendations, with a higher rate of beta-blockers and ACE inhibitors/arb prescription 1. In a selected population with chronic systolic HF (LVEF 35%), Tang et al. 14 have also recently demonstrated cystatin C was associated with poor long-term prognosis. Unlike to this recent study, we studied patients with AHF, including those with preserved LVEF and with a higher rate of co-morbidities, such as hypertension, diabetes mellitus and kidney dysfunction. In the present cohort, we found high cystatin C levels were associated with a higher risk of mortality and/or HF readmission; whereas neither creatinine nor MDRD were significant predictors of adverse events after multivariable adjustment. The
17 highest cystatin C tertile (>1.50 mg/l) was associated with a 3-fold higher risk of adverse events than the lowest cystatin C tertile (<1.04 mg/l). Kaplan-Meier survival analysis showed widely diverging outcomes according to cystatin C tertiles throughout the follow-up period. Lassus et al 15, recently published similar results in a prospective, observational, multicentre study conducted in hospitalized patients with AHF. These authors showed that the prognostic value of cystatin C remained significant after adjustment for established biochemical predictors of adverse events such as creatinine, estimated glomerular filtration rate (Cockcroft Gault), hemoglobin, sodium and NT-proBNP. According to Lassus et al 15, higher cystatin C levels were found in hospitalized patients with AHF than in ambulatory chronic HF patients These findings probably reflect a more advanced kidney dysfunction in patients with AHF resulting in a poor prognosis in this population. In our opinion, since the presence of chronic kidney disease or impaired kidney function during hospitalization have been related to worse outcomes in patients with HF 16-18, the evaluation of kidney function should have a pivotal role in the risk stratification of these patients. Furthermore, we also suggest that cystatin C represents the more useful measure of kidney function for predicting adverse clinical events in this population group. Lassus et al 15, suggested the use of simultaneous cystatin C and NT-proBNP assessment to improve the risk stratification of patients with AHF. Our results not only confirm these earlier findings but also expand on them given that we have also included ctnt in our multimarker risk stratification approach. In this study, we found ctnt level was an important independent predictor of adverse clinical events among hospitalized patients with AHF. Thus, we believe that ctnt should be taken into account in multimarker approaches for risk stratification of these patients. The prognostic value of NT-proBNP is well established, and our results were in accordance with it 5-7. As expected in hospitalized patients with AHF, we found high NT-proBNP concentrations (median 3345 [ ] ng/l) which could also be explained by the older age of the patients and a higher rate of kidney failure in this population. In the
18 present study, we found that each biomarker (cystatin C, NT-proBNP and ctnt) provided independent and complementary prognostic information. By categorizing patients by the number of elevated biomarkers, simultaneous assessment of these 3 biomarkers enabled a powerful prediction of risk of adverse clinical events. Even after adjustment for traditional clinical predictors of adverse events, the prognostic value of the multimarker approach remained significant and was more powerful than the single marker approach. Therefore, our results suggest that a multimarker strategy, with biomarkers combinations targeting various stages of HF development, may allow physicians to identify patients at high risk, who may benefit from closer follow-up and the intensification of proven therapies. The limitations of our study are similar to those of any single centre prospective observational study. The small sample size and relatively small number of patients included in each group also makes it difficult to detect differences across the lower tertiles of cystatin C and to draw firm conclusions. It has been reported that factors other than kidney function, such as corticosteroid use, inflammation, and thyroid function, might influence cystatin C levels 19, 20. However, other studies and metaanalyses 21, 22 have not identified such associations in our population. For the prognosis of outcomes, the number of covariates included in multivariable models was >1 for each 10 outcome events. Therefore, it remains possible that the models were over adjusted. A potential limitation to the multimarker approach is the loss of quantitative information. It should also be acknowledged that elevations in each biomarker may confer different relative risks for individual components of the study endpoint.
19 1.7.1 Table 1. Baseline clinical characteristics according to tertiles of cystatin C. Tertiles Variable 1 st (n=48) 2 nd (n=45) 3 rd (n=45) p Age (years) 72 [56-78] 76 [68-78] 78 [71-84] Men 24 (50%) 27 (60%) 23 (51%) Body mass index, Kg/m 2 28 [25-33] 29 [26-32] 28 [26-31] Systolic blood pressure (mmhg) 149±40 151±32 153± Diastolic blood pressure (mmhg) 86±21 86±20 82± Heart rate (beat/min) 112±30 100±35 101± LVEF 47 [37-60] 49 [30-63] 52 [33-65] NYHA III-IV 11 (23%) 14 (31%) 19 (42%) Chronic heart failure 26 (54%) 29 (64%) 31 (69%) Coronary heart failure 16 (33%) 14 (31%) 18 (40%) Diabetes mellitus 23 (48%) 26 (58%) 21 (47%) Hypertension 37 (79%) 39 (87%) 38 (84%) Hyperlipidemia 16 (33%) 17 (38%) 21 (47%) Current smoking 11 (23%) 7 (16%) 5 (11%) Atrial fibrillation/flutter 27 (59%) 33 (73%) 26 (58%) Branch block 13 (27%) 16 (36%) 13 (29%) Previous STEMI 10 (21%) 8 (18%) 18 (40%) Previous stroke 7 (15%) 9 (20%) 6 (13%) Anemia 15 (31%) 18 (40%) 31 (69%) Chronic Obstructive Pulmonary Disease 3 (6%) 7 (16%) 8 (18%) In-hospital inotropic use 3 (6%) 4 (9%) 12 (27%) Treatment at discharge Beta-blockers ACE inhibitors/arb Statins Spironolactone/Eplerenone Loop diuretics 31 (66%) 40 (84%) 25 (53%) 18 (38%) 43 (91%) 26 (59%) 41 (91%) 24 (54%) 18 (41%) 41 (93%) 17 (44%) 35 (85%) 22 (56%) 11 (28%) 38 (97%) Follow up (days) 289 [ ] 261 [ ] 198 [ ] Data are expressed as mean±sd or median (quartiles), and number (%). LVEF denotes left ventricular ejection fraction, STEMI denotes ST segment elevation myocardial infarction, NYHA denotes New York Heart Association, ACE denotes angiotensinconverting enzyme and ARB denotes angiotensin-receptor blocker.
20 1.7.2 Table 2. Laboratory parameters according to tertiles of cystatin C. Variable 1 st (n=48) Tertiles 2 nd (n=45) 3 rd (n=45) Hemoglobin (g/dl) 13.4± ± ±1.8 <0.001 Glucose (mg/dl) 181±97 166±79 158± Cystatin (mg/l) 0.86 [ ] 1.21 [ ] 1.85 [ ] <0.001 Creatinine (mg/dl) 0.82 [ ] 1.14 [ ] 1.61 [ ] <0.001 egfr (ml/min/ ) 83.6± ± ±16.8 <0.001 Urea nitrogen (mg/dl) 38 [33-48] 51 [42-64] 79 [54-115] <0.001 Albumin (g/dl) 4.2± ± ± Sodium (meq/l) 139± ± ± Uric acid (mg/dl) 6.4± ± ±2.5 <0.001 C-reactive protein (mg/dl) 0.9 [ ] 0.9 [ ] 1.5 [ ] Troponin T (ng/ml) 0.01 [ ] 0.01 [ ] 0.02 [ ] NT-proBNP (pg/ml) 2358 [ ] 3571 [ ] 5255 [ ] <0.001 Data are expressed as mean±sd or median (quartiles), and number (%).egfr denotes estimated glomerular filtration rate and NTproBNP denotes amino-terminal pro-brain natriuretic peptide. p
21 1.7.3 Table 3. Cox regression risk analysis for predictor of mortality and/or HF readmission. Univariable Multivariable* Variable Hazard Ratio P Hazard Ratio p Age (per year) 1.03 ( ) Hyperlipidemia 1.62 ( ) NYHA III-IV 3.17 ( ) < ( ) <0.001 Diabetes mellitus 1.78 ( ) ( ) Previous STEMI ( ) Anemia 1.69 ( ) Inotropic 2.07 ( ) NT-proBNP (per 100 pg/dl) ( ) ( ) Troponin T (per ng/ml) 2.48 ( ) ( ) Cystatin C (per mg/l) 1.64 ( ) ( ) Creatinine (per mg/dl) 1.55 ( ) egfr (per ml/min/1.73m 2 ) 0.96 ( ) Data are expressed as mean±sd or median (quartiles), and number (%). *Cystatin C (mg/l), creatinine (mg/dl) and egfr (ml/min/1.73m 2 ) were all tested separately and multivariable HR and p for other variables shown from the cystatin C model. Abbreviations as in Tables 1 and 2.
22 1.7.4 Table 4. Kidney function parameters and risk of mortality and/or HF readmission. Tertiles Variable 1 st 2 nd 3 rd p Cystatin C (per mg/l) Range n Unadjusted Hazard Ratio Adjusted Hazard Ratio * Creatinine (per mg/dl) Range in women Range in men n Unadjusted Hazard Ratio Adjusted Hazard Ratio * egfr (per ml/min/ ) Range n Unadjusted Hazard Ratio Adjusted Hazard Ratio * ( ) 1.61 ( ) ( ) 1.62 ( ) ( ) 0.86 ( ) ( ) 3.08 ( ) ( ) 1.76 ( ) ( ) 0.52 ( ) *Adjusted for age, New York Heart Association Functional Classification, diabetes mellitus, hyperlipidemia, previous ST segment elevation myocardial infarction, anemia, in-hospital inotropic use, troponin T and NT-proBNP. Abbreviations as in Table 1 and 2.
23 1.8.1 Figure 1. Kaplan-Meier survival analysis of adverse clinical events related to cystatin C tertiles Figure 2. Adverse clinical events according to the number of elevated biomarkers. *Adjusted for age, New York Heart Association Functional Classification, diabetes mellitus, hyperlipidemia, previous ST segment elevation myocardial infarction, anemia and in-hospital inotropic use.
Dr. Luis Miguel Ruilope Jefe de la Unidad de Hipertensión del Hospital Universitario 12 de Octubre, Madrid CONTINUO CARDIOVASCULAR
 Dr. Luis Miguel Ruilope Jefe de la Unidad de Hipertensión del Hospital Universitario 12 de Octubre, Madrid CONTINUO CARDIOVASCULAR Continuo cardiorrenal RETROCESO Target organ damage Asymptomatic CKD New
Dr. Luis Miguel Ruilope Jefe de la Unidad de Hipertensión del Hospital Universitario 12 de Octubre, Madrid CONTINUO CARDIOVASCULAR Continuo cardiorrenal RETROCESO Target organ damage Asymptomatic CKD New
Hígado bioartificial Revisión sistemática
 CONSEJERÍA DE IGUALDAD, SALUD Y POLÍTICAS SOCIALES AGENCIA DE EVALUACIÓN DE TECNOLOGÍAS SANITARIAS DE ANDALUCÍA (AETSA) Hígado bioartificial Revisión sistemática Informe de evaluación de tecnologías emergentes
CONSEJERÍA DE IGUALDAD, SALUD Y POLÍTICAS SOCIALES AGENCIA DE EVALUACIÓN DE TECNOLOGÍAS SANITARIAS DE ANDALUCÍA (AETSA) Hígado bioartificial Revisión sistemática Informe de evaluación de tecnologías emergentes
Influencia de las dislipemias y de su tratamiento sobre el metabolismo de la glucosa, la función renal y miocárdica
 Influencia de las dislipemias y de su tratamiento sobre el metabolismo de la glucosa, la función renal y miocárdica Dr. Carlos Guijarro Unidad de Medicina Interna Universidad Rey Juan Carlos Dislipemias,
Influencia de las dislipemias y de su tratamiento sobre el metabolismo de la glucosa, la función renal y miocárdica Dr. Carlos Guijarro Unidad de Medicina Interna Universidad Rey Juan Carlos Dislipemias,
RELACIÓN ENTRE LOS NIVELES DE CREATINA CINASA MB Y TROPONINA I CON EL ESTADIO DE ENFERMEDAD RENAL CRÓNICA, CIUDAD HOSPITALARIA DR. ENRIQUE TEJERA.
 RELACIÓN ENTRE LOS NIVELES DE CREATINA CINASA MB Y TROPONINA I CON EL ESTADIO DE ENFERMEDAD RENAL CRÓNICA, CIUDAD HOSPITALARIA DR. ENRIQUE TEJERA. ENERO-MAYO 2015 ii UNIVERSIDAD DE CARABOBO FACULTAD DE
RELACIÓN ENTRE LOS NIVELES DE CREATINA CINASA MB Y TROPONINA I CON EL ESTADIO DE ENFERMEDAD RENAL CRÓNICA, CIUDAD HOSPITALARIA DR. ENRIQUE TEJERA. ENERO-MAYO 2015 ii UNIVERSIDAD DE CARABOBO FACULTAD DE
Floridablanca, Colombia.
 22 Floridablanca, Colombia. El síndrome metabólico afecta alrededor de 25% a 45% de la población colombiana de acuerdo con los criterios diagnósticos propuestos por la Federación Internacional de Diabetes,
22 Floridablanca, Colombia. El síndrome metabólico afecta alrededor de 25% a 45% de la población colombiana de acuerdo con los criterios diagnósticos propuestos por la Federación Internacional de Diabetes,
New Horizonts for the management of Dyslipidemia. LDL-c Less than 70 mg/dl
 New Horizonts for the management of Dyslipidemia. LDL-c Less than 70 mg/dl Luis Masana Vascular Medicine and Metabolic Unit Sant Joan University Hospital Rovira & Virgili University. IISPV CIBERDEM Reus
New Horizonts for the management of Dyslipidemia. LDL-c Less than 70 mg/dl Luis Masana Vascular Medicine and Metabolic Unit Sant Joan University Hospital Rovira & Virgili University. IISPV CIBERDEM Reus
La hipertensión arterial en el 2013: las nuevas guías de la ESH/ESC. Alejandro de la Sierra Hospital Mutua Terrassa
 La hipertensión arterial en el 2013: las nuevas guías de la ESH/ESC Alejandro de la Sierra Hospital Mutua Terrassa Universidad de Barcelona J Hypertens 2013; 31: 1281-1357 Eur Heart J 2013; 34: 2159-2219
La hipertensión arterial en el 2013: las nuevas guías de la ESH/ESC Alejandro de la Sierra Hospital Mutua Terrassa Universidad de Barcelona J Hypertens 2013; 31: 1281-1357 Eur Heart J 2013; 34: 2159-2219
Bucaramanga, Colombia.
 157 Bucaramanga, Colombia. INTRODUCCIÓN: estudios previos reportan la validación y correspondencia, o ambas, del índice tobillo brazo oscilométrico frente al índice tobillo brazo con Doppler, pero este
157 Bucaramanga, Colombia. INTRODUCCIÓN: estudios previos reportan la validación y correspondencia, o ambas, del índice tobillo brazo oscilométrico frente al índice tobillo brazo con Doppler, pero este
Publicaciones de FRENA
 Publicaciones de FRENA 1- Clinical outcome in patients with peripheral artery disease. Results from a prospective registry (FRENA). Eur J Intern Med 2008; 19: 192-197. 2- Secondary prevention of arterial
Publicaciones de FRENA 1- Clinical outcome in patients with peripheral artery disease. Results from a prospective registry (FRENA). Eur J Intern Med 2008; 19: 192-197. 2- Secondary prevention of arterial
Insuficiencia Cardíaca
 Cambios en la Enfermedad Cardiovascular en el último año Implicaciones para la Práctica Clínica Insuficiencia Cardíaca Prof. Domingo A. Pascual Figal Hospital Universitario Virgen de la Arrixaca Facultad
Cambios en la Enfermedad Cardiovascular en el último año Implicaciones para la Práctica Clínica Insuficiencia Cardíaca Prof. Domingo A. Pascual Figal Hospital Universitario Virgen de la Arrixaca Facultad
ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES
 ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES OXALIFE IMPLANTS SURFACE IN SMOKING AND NO SMOKING PATIENTS: A CLINICAL STUDY Autor: Malbos Marisel Director: Ibáñez
ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES OXALIFE IMPLANTS SURFACE IN SMOKING AND NO SMOKING PATIENTS: A CLINICAL STUDY Autor: Malbos Marisel Director: Ibáñez
NGAL COMO PREDICTOR DE INJURIA RENAL AGUDA: LA TROPONINA RENAL?
 Congreso Uruguayo de Patología Clínica NGAL COMO PREDICTOR DE INJURIA RENAL AGUDA: LA TROPONINA RENAL? Prof.Agda. Dra Anna Barindelli Laboratorio de Urgencias y Emergencia Hospital de Clínicas, UdelaR
Congreso Uruguayo de Patología Clínica NGAL COMO PREDICTOR DE INJURIA RENAL AGUDA: LA TROPONINA RENAL? Prof.Agda. Dra Anna Barindelli Laboratorio de Urgencias y Emergencia Hospital de Clínicas, UdelaR
Novedades Terapéuticas en IC. Ivabradina
 Novedades Terapéuticas en IC. Ivabradina Las recomendaciones de las Guías de 1 Práctica Clínica José R. González Juanatey Área Cardiovascular. Hospital Clínico Universitario de Santiago de Compostela Ivabradina
Novedades Terapéuticas en IC. Ivabradina Las recomendaciones de las Guías de 1 Práctica Clínica José R. González Juanatey Área Cardiovascular. Hospital Clínico Universitario de Santiago de Compostela Ivabradina
Tratamiento prolongado antiagregante en subgrupos de pacientes. José F. Díaz, MD, FESC Complejo Hospitalario de Huelva
 Tratamiento prolongado antiagregante en subgrupos de pacientes José F. Díaz, MD, FESC Complejo Hospitalario de Huelva Endpoint (%) Primary Endpoint CV Death,MI,Stroke 15 10 CV Death / MI / Stroke Clopidogrel
Tratamiento prolongado antiagregante en subgrupos de pacientes José F. Díaz, MD, FESC Complejo Hospitalario de Huelva Endpoint (%) Primary Endpoint CV Death,MI,Stroke 15 10 CV Death / MI / Stroke Clopidogrel
SPANISH ORAL LANGUAGE ASSESSMENT. Jill Jegerski Department of Modern Languages April 8, 2011
 SPANISH ORAL LANGUAGE ASSESSMENT Jill Jegerski Department of Modern Languages April 8, 2011 INTRODUCTION Basic Spanish program at CSI Three-course Gen. Ed. sequence: SPN 113, 114, 213 Approximately 800
SPANISH ORAL LANGUAGE ASSESSMENT Jill Jegerski Department of Modern Languages April 8, 2011 INTRODUCTION Basic Spanish program at CSI Three-course Gen. Ed. sequence: SPN 113, 114, 213 Approximately 800
Volatilidad: Noviembre 2010 Futuros Frijol de Soya
 Observaciones Junio 09, 2010 1. La volatilidad tiene una tendencia a aumentar de Junio a Julio. 2. Este reporte sugiere que se debería considerar la implementación de estrategias largas con opciones en
Observaciones Junio 09, 2010 1. La volatilidad tiene una tendencia a aumentar de Junio a Julio. 2. Este reporte sugiere que se debería considerar la implementación de estrategias largas con opciones en
iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain)
 iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain) ! Introduction! Passage Retrieval Systems! IR-n system! IR-n system at iclef-2002! Conclusions and Future works ! Introduction!
iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain) ! Introduction! Passage Retrieval Systems! IR-n system! IR-n system at iclef-2002! Conclusions and Future works ! Introduction!
ESTUDIO COMPARATIVO DE TRES TIPOS DE ESFICMOMANOMETROS, EN SUJETOS CON DIFERENTES CIFRAS DE PRESION ARTERIAL.
 01---- - ESTUDIO COMPARATIVO DE TRES TIPOS DE ESFICMOMANOMETROS, EN SUJETOS CON DIFERENTES CIFRAS DE PRESION ARTERIAL. Victorio Fernandez Gorcfa~ Mtra. Rosa A Zarate Grajales** *Pasante de LicenClatura
01---- - ESTUDIO COMPARATIVO DE TRES TIPOS DE ESFICMOMANOMETROS, EN SUJETOS CON DIFERENTES CIFRAS DE PRESION ARTERIAL. Victorio Fernandez Gorcfa~ Mtra. Rosa A Zarate Grajales** *Pasante de LicenClatura
UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda
 UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda EVALUACIÓN IN VITRO DE LA FILTRACIÓN APICAL EN RAICES DE DIENTES EXTRAIDOS, UTILIZANDO DOS MÉTODOS DE OBTURACION:
UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda EVALUACIÓN IN VITRO DE LA FILTRACIÓN APICAL EN RAICES DE DIENTES EXTRAIDOS, UTILIZANDO DOS MÉTODOS DE OBTURACION:
UPV software for risk models
 UPV software for risk models Armando Serrano Lombillo arserlom@doctor.upv.es www.edams.upv.es Risk analysis is feasible 1 Contents Introduction Review of previous concepts From influence diagrams to event
UPV software for risk models Armando Serrano Lombillo arserlom@doctor.upv.es www.edams.upv.es Risk analysis is feasible 1 Contents Introduction Review of previous concepts From influence diagrams to event
UNIVERSIDAD NACIONAL DE INGENIERIA
 i UNIVERSIDAD NACIONAL DE INGENIERIA ESCUELA UNIVERSITARIA DE POSTGRADO MAESTRIA EN GESTIÓN AMBIENTAL ASPECTOS SANITARIOS EN EL SISTEMA DE ABASTECIMIENTO DE AGUA POTABLE MEDIANTE CAMIONES CISTERNAS EN
i UNIVERSIDAD NACIONAL DE INGENIERIA ESCUELA UNIVERSITARIA DE POSTGRADO MAESTRIA EN GESTIÓN AMBIENTAL ASPECTOS SANITARIOS EN EL SISTEMA DE ABASTECIMIENTO DE AGUA POTABLE MEDIANTE CAMIONES CISTERNAS EN
El NT- pro BNP en Medicina Interna. Elena Rodríguez Castellano
 El NT- pro BNP en Medicina Interna Elena Rodríguez Castellano R4 Medicina Interna Qué es el NT probnp? Antagonistas naturales del sistema RAA y del Sistema Nervioso Simpático. Utilidad del NT-proBNP Diagnóstico
El NT- pro BNP en Medicina Interna Elena Rodríguez Castellano R4 Medicina Interna Qué es el NT probnp? Antagonistas naturales del sistema RAA y del Sistema Nervioso Simpático. Utilidad del NT-proBNP Diagnóstico
Caso clínico: Mujer diabética de 82 años
 Caso clínico: Mujer diabética de 82 años José Manuel Millaruelo Trillo Centro de Salud Torrero La Paz. Zaragoza Reunión GEDAPS Barcelona 6 de Noviembre 2009 Posibles enfoques Encorsetarla en los objetivos
Caso clínico: Mujer diabética de 82 años José Manuel Millaruelo Trillo Centro de Salud Torrero La Paz. Zaragoza Reunión GEDAPS Barcelona 6 de Noviembre 2009 Posibles enfoques Encorsetarla en los objetivos
"Average years of healthy life (without disabilities). Argentina 2002-2003.
 Universidad Nacional de Córdoba "Average years of healthy life (without disabilities). Argentina 2002-2003. Alvarez, M. - Carrizo, E. - Peláez, E. - González, L. CONICET - National University of Córdoba,
Universidad Nacional de Córdoba "Average years of healthy life (without disabilities). Argentina 2002-2003. Alvarez, M. - Carrizo, E. - Peláez, E. - González, L. CONICET - National University of Córdoba,
Terapia de campo de tumores en el tratamiento del glioblastoma
 Terapia de campo de tumores en el tratamiento del glioblastoma Revisión sistemática Informe de síntesis de tecnología emergente Tumor treating fields therapy (TTF) for glioblastoma. A Systematic Review
Terapia de campo de tumores en el tratamiento del glioblastoma Revisión sistemática Informe de síntesis de tecnología emergente Tumor treating fields therapy (TTF) for glioblastoma. A Systematic Review
ARIS Solution for Governance, Risk & Compliance Management. Ensure Business Compliance
 ARIS Solution for Governance, Risk & Compliance Management Ensure Business Compliance El exito en la implementacion de GRC consiste en mantener el balance correcto 7 June 2012 Software AG - Get There Faster
ARIS Solution for Governance, Risk & Compliance Management Ensure Business Compliance El exito en la implementacion de GRC consiste en mantener el balance correcto 7 June 2012 Software AG - Get There Faster
Objetivo: Investigar los cambios ocurridos en la epidemiología clínica y molecular de A. baumannii entre 2000 y Método: Dos estudios
 1 2 3 and the GEIH/GEMARA/REIPI-Ab2010 Group. 4 Objetivo: Investigar los cambios ocurridos en la epidemiología clínica y molecular de A. baumannii entre 2000 y 2010. Método: Dos estudios prospectivos de
1 2 3 and the GEIH/GEMARA/REIPI-Ab2010 Group. 4 Objetivo: Investigar los cambios ocurridos en la epidemiología clínica y molecular de A. baumannii entre 2000 y 2010. Método: Dos estudios prospectivos de
Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo
 The American College of Obstetricians and Gynecologists WOMEN S HEALTH CARE PHYSICIANS Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo NOTA: Esta es una traducción libre realizada con la
The American College of Obstetricians and Gynecologists WOMEN S HEALTH CARE PHYSICIANS Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo NOTA: Esta es una traducción libre realizada con la
La EPOC como factor de riesgo para Cáncer de Pulmón. Dr. Juan Pablo de Torres Tajes Servicio de Neumología Clínica Universidad de Navarra
 La EPOC como factor de riesgo para Cáncer de Pulmón Dr. Juan Pablo de Torres Tajes Servicio de Neumología Clínica Universidad de Navarra Resumen Una asociación letal Nuestros datos Posibles mecanismos
La EPOC como factor de riesgo para Cáncer de Pulmón Dr. Juan Pablo de Torres Tajes Servicio de Neumología Clínica Universidad de Navarra Resumen Una asociación letal Nuestros datos Posibles mecanismos
Pregunta 1 Suponga que una muestra de 35 observaciones es obtenida de una población con media y varianza. Entonces la se calcula como.
 Universidad de Costa Rica Programa de Posgrado en Computación e Informática Doctorado en Computación e Informática Curso Estadística 18 de febrero 2013 Nombre: Segundo examen corto de Probabilidad Pregunta
Universidad de Costa Rica Programa de Posgrado en Computación e Informática Doctorado en Computación e Informática Curso Estadística 18 de febrero 2013 Nombre: Segundo examen corto de Probabilidad Pregunta
Análisis de la coestimulación vía CD28 en células linfoides de pacientes infectados. con el virus de la Hepatitis C RESUMEN
 Análisis de la coestimulación vía CD28 en células linfoides de pacientes infectados con el virus de la Hepatitis C RESUMEN La infección por el virus de la hepatitis C (VHC) afecta a más de 170 millones
Análisis de la coestimulación vía CD28 en células linfoides de pacientes infectados con el virus de la Hepatitis C RESUMEN La infección por el virus de la hepatitis C (VHC) afecta a más de 170 millones
OBJETIVO: determinar la incidencia de trombosis de stents liberadores y no liberadores de medicamento en pacientes del «mundo real».
 99 Bogotá, DC., Colombia. ANTECEDENTES: la evidencia disponible de stents liberadores de medicamento proviene de estudios controlados con estrictos criterios de inclusión, limitando sus conclusiones y
99 Bogotá, DC., Colombia. ANTECEDENTES: la evidencia disponible de stents liberadores de medicamento proviene de estudios controlados con estrictos criterios de inclusión, limitando sus conclusiones y
COMPARACIÓN DE LA CALIDAD DE VIDA RELACIONADA CON LA SALUD EN
 Escuela Universitaria de Enfermería TRABAJO FIN DE GRADO COMPARACIÓN DE LA CALIDAD DE VIDA RELACIONADA CON LA SALUD EN PACIENTES CON HIPERTENSIÓN ARTERIAL Y PACIENTES CON DIABETES MELLITUS Pilar Irene
Escuela Universitaria de Enfermería TRABAJO FIN DE GRADO COMPARACIÓN DE LA CALIDAD DE VIDA RELACIONADA CON LA SALUD EN PACIENTES CON HIPERTENSIÓN ARTERIAL Y PACIENTES CON DIABETES MELLITUS Pilar Irene
Ignacio Ferreira González. Unidad de Epidemiología. Servicio de Cardiología. Hospital Vall d Hebron. Barcelona.
 Ignacio Ferreira González. Unidad de Epidemiología. Servicio de Cardiología. Hospital Vall d Hebron. Barcelona. Variables de resultado combinadas en los ensayos clínicos (Composite Endpoint / Composite
Ignacio Ferreira González. Unidad de Epidemiología. Servicio de Cardiología. Hospital Vall d Hebron. Barcelona. Variables de resultado combinadas en los ensayos clínicos (Composite Endpoint / Composite
Este proyecto tiene como finalidad la creación de una aplicación para la gestión y explotación de los teléfonos de los empleados de una gran compañía.
 SISTEMA DE GESTIÓN DE MÓVILES Autor: Holgado Oca, Luis Miguel. Director: Mañueco, MªLuisa. Entidad Colaboradora: Eli & Lilly Company. RESUMEN DEL PROYECTO Este proyecto tiene como finalidad la creación
SISTEMA DE GESTIÓN DE MÓVILES Autor: Holgado Oca, Luis Miguel. Director: Mañueco, MªLuisa. Entidad Colaboradora: Eli & Lilly Company. RESUMEN DEL PROYECTO Este proyecto tiene como finalidad la creación
OSH: Integrated from school to work.
 SST: Integrada desde la escuela hasta el empleo. OSH: Integrated from school to work. ESPAÑA - SPAIN Mª Mercedes Tejedor Aibar José Luis Castellá López Instituto Nacional de Seguridad e Higiene en el Trabajo
SST: Integrada desde la escuela hasta el empleo. OSH: Integrated from school to work. ESPAÑA - SPAIN Mª Mercedes Tejedor Aibar José Luis Castellá López Instituto Nacional de Seguridad e Higiene en el Trabajo
DEDICATORIA. A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día.
 DEDICATORIA A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día. A mi hermano, que me motiva a seguir siempre adelante. A mi esposo, por estar a mi lado y brindarme
DEDICATORIA A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día. A mi hermano, que me motiva a seguir siempre adelante. A mi esposo, por estar a mi lado y brindarme
Bystander effect. Amy Lozano White Radiology and physical medicine Year 4 of Medicine Studies
 Bystander effect Amy Lozano White Radiology and physical medicine Year 4 of Medicine Studies Key points Concept Historical evolution Paradigm change Mechanisms Its implications in radiological protection
Bystander effect Amy Lozano White Radiology and physical medicine Year 4 of Medicine Studies Key points Concept Historical evolution Paradigm change Mechanisms Its implications in radiological protection
Bactrocera oleae (Gmelin) (Díptera: Tephritidae), pero dado el poco rendimiento de nuestra población mantenida en laboratorio, se tomó como modelo la
 RESUMEN El primer objetivo de este trabajo fue aislamiento cepas de hongos entomopatógenos a partir de suelo de olivar de Andalucía (España).El método de la " trampa Gallería" permitió identificar y aislar
RESUMEN El primer objetivo de este trabajo fue aislamiento cepas de hongos entomopatógenos a partir de suelo de olivar de Andalucía (España).El método de la " trampa Gallería" permitió identificar y aislar
Paradoja de la Obesidad
 Paradoja de la Obesidad Francisco J. Pasquel, MD Assistant Professor of Medicine Emory University School of Medicine Director, Endocrine Clinic Grady Health System Definición La obesidad se asocia con
Paradoja de la Obesidad Francisco J. Pasquel, MD Assistant Professor of Medicine Emory University School of Medicine Director, Endocrine Clinic Grady Health System Definición La obesidad se asocia con
Certificación en España según normas UNE-EN-ISO 9000 y 14000
 Certificación en España según normas UNE-EN-ISO 9000 y 14000 Sexto informe de Forum Calidad Es este el sexto informe que Forum Calidad presenta sobre el número y distribución de las organizaciones españolas
Certificación en España según normas UNE-EN-ISO 9000 y 14000 Sexto informe de Forum Calidad Es este el sexto informe que Forum Calidad presenta sobre el número y distribución de las organizaciones españolas
Patters of evolution of the Mexican clearing house system (1940-1980) Demography or Levels of Economic Activity? Gustavo A.
 Patters of evolution of the Mexican clearing house system (1940-1980) Demography or Levels of Economic Activity? Gustavo A. Del Angel 2 Some facts for the period 1940-1980: Between the 1940s and the late
Patters of evolution of the Mexican clearing house system (1940-1980) Demography or Levels of Economic Activity? Gustavo A. Del Angel 2 Some facts for the period 1940-1980: Between the 1940s and the late
PROGRAMA. Operaciones de Banca y Bolsa SYLLABUS BANKING AND STOCK MARKET OPERATIONS
 PROGRAMA 4º Curso. Grado en Administración y Dirección SYLLABUS BANKING AND STOCK MARKET OPERATIONS 4 rd year. Pág. 1 / 8 Colegio Universitario de Estudios Financieros Leonardo Prieto Castro, 2 Tel. +34
PROGRAMA 4º Curso. Grado en Administración y Dirección SYLLABUS BANKING AND STOCK MARKET OPERATIONS 4 rd year. Pág. 1 / 8 Colegio Universitario de Estudios Financieros Leonardo Prieto Castro, 2 Tel. +34
Personal Dosimetry Statistics and Specifics of Low Dose Evaluation
 Personal Dosimetry Statistics and Specifics of Low Dose Evaluation Comisión Chilena de Energía Nuclear Ricardo Avila, Roberto Gómez, Personal Dosimetry Laboratory and Carlos Oyarzún, Metrology of Ionizing
Personal Dosimetry Statistics and Specifics of Low Dose Evaluation Comisión Chilena de Energía Nuclear Ricardo Avila, Roberto Gómez, Personal Dosimetry Laboratory and Carlos Oyarzún, Metrology of Ionizing
ITHACA TELEMEDICINE SERVICE FOR CHRONIC HYPERTENSIVE PATIENTS
 ITHACA TELEMEDICINE SERVICE FOR CHRONIC HYPERTENSIVE PATIENTS Population risk stratification in chronic complex patients: from the strategy to an attention model Antoni Sicras Mainar MD PhD Head of Innovation
ITHACA TELEMEDICINE SERVICE FOR CHRONIC HYPERTENSIVE PATIENTS Population risk stratification in chronic complex patients: from the strategy to an attention model Antoni Sicras Mainar MD PhD Head of Innovation
2 INFORMES, ESTUDIOS E INVESTIGACIÓN
 2 INFORMES, ESTUDIOS E INVESTIGACIÓN Efectos de los factores de crecimiento tisular tras la resección mayor del hígado. Effects of tissue growth factors after major liver resection. Executive summary.
2 INFORMES, ESTUDIOS E INVESTIGACIÓN Efectos de los factores de crecimiento tisular tras la resección mayor del hígado. Effects of tissue growth factors after major liver resection. Executive summary.
Cambridge IGCSE. www.cie.org.uk
 Cambridge IGCSE About CIE CIE examinations are taken in over 125 different countries Cambridge qualifications are recognised by universities, colleges and employers across the globe Sobre CIE Los exámenes
Cambridge IGCSE About CIE CIE examinations are taken in over 125 different countries Cambridge qualifications are recognised by universities, colleges and employers across the globe Sobre CIE Los exámenes
SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México
 SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México How did started the Safety Road Show? Airbus Helicopters and others manufacturers did invest since a long time in improving Aviation Safety. In
SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México How did started the Safety Road Show? Airbus Helicopters and others manufacturers did invest since a long time in improving Aviation Safety. In
Diseño de un directorio Web de diseñadores gráficos, ilustradores y fotógrafos.
 Universidad Nueva Esparta Facultad de Ciencias Administrativas Escuela de Administración de Diseño de un directorio Web de diseñadores gráficos, ilustradores y fotógrafos. Tutor: Lic. Beaujon, María Beatriz
Universidad Nueva Esparta Facultad de Ciencias Administrativas Escuela de Administración de Diseño de un directorio Web de diseñadores gráficos, ilustradores y fotógrafos. Tutor: Lic. Beaujon, María Beatriz
UNIT 9.- INTRODUCTION TO HYPOTHESIS TESTING.
 STATISTICAL METHODS FOR BUSINESS UNIT 9.- INTRODUCTION TO HYPOTHESIS TESTING. 9.1.- Basics of statistical hypothesis testing. 9.2.- Types of errors in hypothesis testing. 9.3.- Methodology and implementation
STATISTICAL METHODS FOR BUSINESS UNIT 9.- INTRODUCTION TO HYPOTHESIS TESTING. 9.1.- Basics of statistical hypothesis testing. 9.2.- Types of errors in hypothesis testing. 9.3.- Methodology and implementation
Consejería de Salud Agencia de Evaluación de Tecnologías Sanitarias de Andalucía
 CONSEJERÍA DE SALUD Coste-efectividad del palivizumab en la prevención de la hospitalización por virus respiratorio sincitial en prematuros de 32 a 35 semanas de gestación. Actualización del informe 5
CONSEJERÍA DE SALUD Coste-efectividad del palivizumab en la prevención de la hospitalización por virus respiratorio sincitial en prematuros de 32 a 35 semanas de gestación. Actualización del informe 5
PEMEX E&P South Region OMC 2015
 PEMEX E&P South Region OMC 2015 Austin, TX. USA Por: Mario Alejandro Mosqueda Thompson (PEMEX) Juan D. Osorio Monsalve (OVS GROUP MEXICO) The system is based on integrating databases and capture of different
PEMEX E&P South Region OMC 2015 Austin, TX. USA Por: Mario Alejandro Mosqueda Thompson (PEMEX) Juan D. Osorio Monsalve (OVS GROUP MEXICO) The system is based on integrating databases and capture of different
Investigación Clínica
 Investigación Clínica Intervención vs No Intervención Ensayo Clínico Controlado Análisis de Registros Dr. José Ramón Paniagua Sierra División de Desarrollo de la Investigación Coordinación de Investigación
Investigación Clínica Intervención vs No Intervención Ensayo Clínico Controlado Análisis de Registros Dr. José Ramón Paniagua Sierra División de Desarrollo de la Investigación Coordinación de Investigación
GENERAL INFORMATION Project Description
 RESULTADOS! GENERAL INFORMATION Project Description The campaign "Adopt a car " had as its main objective to position Autoplaza, the main automotive selling point of Chile, as a new car sales location
RESULTADOS! GENERAL INFORMATION Project Description The campaign "Adopt a car " had as its main objective to position Autoplaza, the main automotive selling point of Chile, as a new car sales location
Final Project (academic investigation)
 Final Project (academic investigation) MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Final Project (academic
Final Project (academic investigation) MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Final Project (academic
Ús de les estatines en els/les pacients d alt risc cardiovascular
 Ús de les estatines en els/les pacients d alt risc cardiovascular Lluís Masana Unitat de Lípids Catalunya Sud. Hospitals Reus, Tarragona, Tortosa, Valls, Vendrell. Universitat Rovira i Virgili. IISPV.
Ús de les estatines en els/les pacients d alt risc cardiovascular Lluís Masana Unitat de Lípids Catalunya Sud. Hospitals Reus, Tarragona, Tortosa, Valls, Vendrell. Universitat Rovira i Virgili. IISPV.
ESTUDIO OBINDIAB GRUPO DE DIABETES SEMFYC
 ESTUDIO OBINDIAB GRUPO DE DIABETES SEMFYC METHODS CHARACTERISTICS OF THE PATIENTS Mean (SD) Range CI95% Age (years) 68,9+11,3 40-95 (67,8-70,0) HbA1c (%) 6,97+1,2 5,0-14,7 (6,9-7,1) Gender Male Female
ESTUDIO OBINDIAB GRUPO DE DIABETES SEMFYC METHODS CHARACTERISTICS OF THE PATIENTS Mean (SD) Range CI95% Age (years) 68,9+11,3 40-95 (67,8-70,0) HbA1c (%) 6,97+1,2 5,0-14,7 (6,9-7,1) Gender Male Female
Introducción al CDA Clinical Document Architecture
 Con la colaboración de: Introducción al CDA Clinical Document Architecture Josep Vilalta Marzo www.vico.org Universitat Internacional de Catalunya Madrid 25 de Mayo de 2004 1 Madrid 25 de Mayo de 2004
Con la colaboración de: Introducción al CDA Clinical Document Architecture Josep Vilalta Marzo www.vico.org Universitat Internacional de Catalunya Madrid 25 de Mayo de 2004 1 Madrid 25 de Mayo de 2004
José María Hernández
 José María Hernández 1.Introduction 2.PARTNER Trials 3.COREVALVE Trials 4.Current Guidelines 5.Intermediate Risk 6.Low Risk 7.Conclusions < 2008 21 34 Rigorous Clinical Research PubMed annual number TAVI
José María Hernández 1.Introduction 2.PARTNER Trials 3.COREVALVE Trials 4.Current Guidelines 5.Intermediate Risk 6.Low Risk 7.Conclusions < 2008 21 34 Rigorous Clinical Research PubMed annual number TAVI
Pruebas genómicas para el pronóstico de pacientes con cáncer de mama. MammaPrint y Oncotype DX
 Pruebas genómicas para el pronóstico de pacientes con cáncer de mama. MammaPrint y Oncotype DX Prognostic genomic tests in early breast: MammaPrint and Oncotype DX. Executive summary INFORMES DE EVALUACIÓN
Pruebas genómicas para el pronóstico de pacientes con cáncer de mama. MammaPrint y Oncotype DX Prognostic genomic tests in early breast: MammaPrint and Oncotype DX. Executive summary INFORMES DE EVALUACIÓN
REVASCULARIZACION MIOCARDICA MULTIPLES VASOS Y TRONCO
 REVASCULARIZACION MIOCARDICA MULTIPLES VASOS Y TRONCO Congreso Federacion Argentina de Cardiologia 29 31 Mayo 2014 Mendoza Dr. Eduardo Hasbani CABG vs PCI con DES COMO REVASCULARIZAR? DR EDUARDO HASBANI
REVASCULARIZACION MIOCARDICA MULTIPLES VASOS Y TRONCO Congreso Federacion Argentina de Cardiologia 29 31 Mayo 2014 Mendoza Dr. Eduardo Hasbani CABG vs PCI con DES COMO REVASCULARIZAR? DR EDUARDO HASBANI
La mortalidad inmediata total fue de 3,3%. La frecuencia de mortalidad para los grupos fue de 6,5% (n= 6) vs. 1,9% (n= 4) respectivamente.
 33 Bogotá, Colombia. Existen controversias acerca de las posibles ventajas del abordaje transperitoneal vs. extraperitoneal en la cirugía de aneurisma de aorta abdominal; con este último, algunos estudios
33 Bogotá, Colombia. Existen controversias acerca de las posibles ventajas del abordaje transperitoneal vs. extraperitoneal en la cirugía de aneurisma de aorta abdominal; con este último, algunos estudios
Cromatografía líquida desnaturalizante de alto rendimiento (DHPLC)
 Cromatografía líquida desnaturalizante de alto rendimiento (DHPLC) Uso y utilidad en el genotipado masivo Denaturing high performance liquid chromatography (DHPLC). Use and utility in massive genotyping.
Cromatografía líquida desnaturalizante de alto rendimiento (DHPLC) Uso y utilidad en el genotipado masivo Denaturing high performance liquid chromatography (DHPLC). Use and utility in massive genotyping.
PERSISTENT ORGANIC COMPOUNDS (POC S) ARE VERY TOXIC AND THEY PROVOKE DISEASES LIKE: -- Genetics damage from the birth.
 1 COMPARATIVE STUDY OF THE BIOACUMULATION OF POC S AND GENETIC DAMAGE IN LIVER OF Goodea atripinnis FISH And THE PELECAN Pelicanus erythrorhyncus OF THE LAKE OF CHAPALA AND OF THE LAGOON OF SAYULA According
1 COMPARATIVE STUDY OF THE BIOACUMULATION OF POC S AND GENETIC DAMAGE IN LIVER OF Goodea atripinnis FISH And THE PELECAN Pelicanus erythrorhyncus OF THE LAKE OF CHAPALA AND OF THE LAGOON OF SAYULA According
Centro Oficial de Trinity College London Desde 1989 el Instituto Dickens representa a Trinity College London en el Uruguay.
 Dickens Institute Centro Oficial de Trinity College London Desde 1989 el Instituto Dickens representa a Trinity College London en el Uruguay. Este centro de Exámenes Internacionales, reconocido en más
Dickens Institute Centro Oficial de Trinity College London Desde 1989 el Instituto Dickens representa a Trinity College London en el Uruguay. Este centro de Exámenes Internacionales, reconocido en más
Dr. Lobo. H Txagorritxu Dr. Nieto. H Virgen de la Luz Dr. Monreal. H Trias i Pujol
 Dr. Lobo. H Txagorritxu Dr. Nieto. H Virgen de la Luz Dr. Monreal. H Trias i Pujol Hemiplejía por HIC (15 d) Disnea y datos de TVP .. Data on treatment of VTE in patients with intracranial hemorrhage are
Dr. Lobo. H Txagorritxu Dr. Nieto. H Virgen de la Luz Dr. Monreal. H Trias i Pujol Hemiplejía por HIC (15 d) Disnea y datos de TVP .. Data on treatment of VTE in patients with intracranial hemorrhage are
Impacto de los factores de riesgo cardiovascular tradicionales en el lupus eritematoso sistémico
 Impacto de los factores de riesgo cardiovascular tradicionales en el lupus eritematoso sistémico Dr. José Mario Sabio UEAS. Servicio de Medicina Interna. Hospital Universitario Virgen de la Nieves. Granada.
Impacto de los factores de riesgo cardiovascular tradicionales en el lupus eritematoso sistémico Dr. José Mario Sabio UEAS. Servicio de Medicina Interna. Hospital Universitario Virgen de la Nieves. Granada.
UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR.
 UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR. Autor: Ruiz Muñoz, Rafael. Director: Muñoz García, Manuel. Entidad Colaboradora: Empresarios Agrupados.
UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR. Autor: Ruiz Muñoz, Rafael. Director: Muñoz García, Manuel. Entidad Colaboradora: Empresarios Agrupados.
IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR
 IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR Subject: Important Updates Needed for Your FAFSA Dear [Applicant], When you completed your 2012-2013 Free Application for Federal Student Aid
IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR Subject: Important Updates Needed for Your FAFSA Dear [Applicant], When you completed your 2012-2013 Free Application for Federal Student Aid
MANUAL EASYCHAIR. A) Ingresar su nombre de usuario y password, si ya tiene una cuenta registrada Ó
 MANUAL EASYCHAIR La URL para enviar su propuesta a la convocatoria es: https://easychair.org/conferences/?conf=genconciencia2015 Donde aparece la siguiente pantalla: Se encuentran dos opciones: A) Ingresar
MANUAL EASYCHAIR La URL para enviar su propuesta a la convocatoria es: https://easychair.org/conferences/?conf=genconciencia2015 Donde aparece la siguiente pantalla: Se encuentran dos opciones: A) Ingresar
Es la Diabetes una Enfermedad CVC?
 Es la Diabetes una Enfermedad CVC? 1 Sin duda que SI 1 José R. González Juanatey Área Cardiovascular. Hospital Clínico Universitario de Santiago de Compostela Es la Diabetes una ECV? Lo es en el Diagnóstico?
Es la Diabetes una Enfermedad CVC? 1 Sin duda que SI 1 José R. González Juanatey Área Cardiovascular. Hospital Clínico Universitario de Santiago de Compostela Es la Diabetes una ECV? Lo es en el Diagnóstico?
INSTRUCTIONS FOR COMPLETING THE UA_SGE_FT_03_FI_IE FORM REGARDING NATURAL PERSONS DATA FOR THE UA SUPPLIERS DATABASE
 INSTRUCTIONS FOR COMPLETING THE UA_SGE_FT_03_FI_IE FORM REGARDING NATURAL PERSONS DATA FOR THE UA SUPPLIERS DATABASE This form is for use by both Spanish and foreign natural persons. Due to the new requirements
INSTRUCTIONS FOR COMPLETING THE UA_SGE_FT_03_FI_IE FORM REGARDING NATURAL PERSONS DATA FOR THE UA SUPPLIERS DATABASE This form is for use by both Spanish and foreign natural persons. Due to the new requirements
INDICACIÓN DE INTERVENCIÓN. Indicaciones de Valvuloplastía Mitral Percutanea con Balón. Indicaciones de Valvulopastia Mitral Quirúrgica
 INDICACIÓN DE INTERVENCIÓN Indicaciones de Valvuloplastía Mitral Percutanea con Balón Indicaciones de Valvulopastia Mitral Quirúrgica Indicaciones de Reemplazo Valvular INDICACIÓN DE INTERVENCIÓN Pacientes
INDICACIÓN DE INTERVENCIÓN Indicaciones de Valvuloplastía Mitral Percutanea con Balón Indicaciones de Valvulopastia Mitral Quirúrgica Indicaciones de Reemplazo Valvular INDICACIÓN DE INTERVENCIÓN Pacientes
ACTIVITIES 2014 CHILEAN MINING COMMISSION
 ACTIVITIES 2014 CHILEAN MINING COMMISSION Santiago, June 2014 Overview Introduction Organizations Main Events - year 2014 Some Details Constitution of the Board The current Board is constituted, composed
ACTIVITIES 2014 CHILEAN MINING COMMISSION Santiago, June 2014 Overview Introduction Organizations Main Events - year 2014 Some Details Constitution of the Board The current Board is constituted, composed
Desventajas Requiere un grado de motivación y de atención a la limpieza mientras se realizan los intercambios.
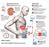 === Ventajas === * Puede hacerse en casa. * Relativamente fácil de aprender. * Fácil para viajar, los bolsos de solución son fáciles de llevar en vacaciones. * El balance de fluido es normalmente más fácil
=== Ventajas === * Puede hacerse en casa. * Relativamente fácil de aprender. * Fácil para viajar, los bolsos de solución son fáciles de llevar en vacaciones. * El balance de fluido es normalmente más fácil
Trading & Investment In Banking
 Trading & Investment In Banking MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Trading & Investment In
Trading & Investment In Banking MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Trading & Investment In
Matemáticas Muestra Cuadernillo de Examen
 Matemáticas Muestra Cuadernillo de Examen Papel-Lápiz Formato Estudiante Español Versión, Grados 3-5 Mathematics Sample Test Booklet Paper-Pencil Format Student Spanish Version, Grades 3 5 Este cuadernillo
Matemáticas Muestra Cuadernillo de Examen Papel-Lápiz Formato Estudiante Español Versión, Grados 3-5 Mathematics Sample Test Booklet Paper-Pencil Format Student Spanish Version, Grades 3 5 Este cuadernillo
Kegel exercises spanish pdf
 Kegel exercises spanish pdf not do this as an exercise on the toilet. HEALTH EDUCATION. Kegels: Pelvic Floor Strengthening. Exercises for Women. What are pelvic floor muscles? 30 Jun 2017. Los músculos
Kegel exercises spanish pdf not do this as an exercise on the toilet. HEALTH EDUCATION. Kegels: Pelvic Floor Strengthening. Exercises for Women. What are pelvic floor muscles? 30 Jun 2017. Los músculos
Efecto de las nubes magnéticas sobre la propagación de los rayos cósmicos
 Efecto de las nubes magnéticas sobre la propagación de los rayos cósmicos J.J. Blanco, M.A. Hidalgo, J. Rodríguez-Pacheco, J. Medina y D. Arrazola Space Research Group, Universidad de Alcalá (Spain) Helios
Efecto de las nubes magnéticas sobre la propagación de los rayos cósmicos J.J. Blanco, M.A. Hidalgo, J. Rodríguez-Pacheco, J. Medina y D. Arrazola Space Research Group, Universidad de Alcalá (Spain) Helios
The Home Language Survey (HLS) and Identification of Students
 The Home Language Survey (HLS) and Identification of Students The Home Language Survey (HLS) is the document used to determine a student that speaks a language other than English. Identification of a language
The Home Language Survey (HLS) and Identification of Students The Home Language Survey (HLS) is the document used to determine a student that speaks a language other than English. Identification of a language
T R A N S TECHNICAL SPECIFICATIONS:
 A R P O L T R A N S TECHNICAL SPECIFICATIONS: 1, or - look casing Specially designed rubber gasket (various models) Steps of up tc 8 mm between outside diameters Working pressures up to bar F l e x i b
A R P O L T R A N S TECHNICAL SPECIFICATIONS: 1, or - look casing Specially designed rubber gasket (various models) Steps of up tc 8 mm between outside diameters Working pressures up to bar F l e x i b
Identificación rápida de Staphylococcus aureus meticilina resistente Cribado de portadores
 Identificación rápida de Staphylococcus aureus meticilina resistente Cribado de portadores Informe de síntesis de tecnologías emergentes Rapid tests for methicillin resistant Staphylococcus aureus. Carrier
Identificación rápida de Staphylococcus aureus meticilina resistente Cribado de portadores Informe de síntesis de tecnologías emergentes Rapid tests for methicillin resistant Staphylococcus aureus. Carrier
Efficacy, safety and efficiency of transcutaneous nerve stimulation for the treatment of chronic musculoskeletal pain.
 Eficacia, seguridad y coste-efectividad de la estimulación nerviosa eléctrica transcutánea (TENS) en el tratamiento del dolor musculoesquelético crónico Efficacy, safety and efficiency of transcutaneous
Eficacia, seguridad y coste-efectividad de la estimulación nerviosa eléctrica transcutánea (TENS) en el tratamiento del dolor musculoesquelético crónico Efficacy, safety and efficiency of transcutaneous
IE12_ CONSOLIDACIÓN Y DESARROLLO DE NUEVAS TÉCNICAS DE EVALUACIÓN INTENSIVAS ON-LINE YA IMPLEMENTADAS POR EL GIE E4
 IE12_13-03001 - CONSOLIDACIÓN Y DESARROLLO DE NUEVAS TÉCNICAS DE EVALUACIÓN Departamento de Estructuras de la Edificación Escuela Técnica Superior de Arquitectura de Madrid Universidad Politécnica de Madrid
IE12_13-03001 - CONSOLIDACIÓN Y DESARROLLO DE NUEVAS TÉCNICAS DE EVALUACIÓN Departamento de Estructuras de la Edificación Escuela Técnica Superior de Arquitectura de Madrid Universidad Politécnica de Madrid
Dr. León Valdivieso Staff. Dpto de Cardiología Intervencionista. Fundación Favaloro
 TAVI Complicaciones periprocedimiento. Impacto en la evolución Dr. León Valdivieso Staff. Dpto de Cardiología Intervencionista Conflictos de Intereses: Ninguno relacionado a esta presentación. LBBB Stroke
TAVI Complicaciones periprocedimiento. Impacto en la evolución Dr. León Valdivieso Staff. Dpto de Cardiología Intervencionista Conflictos de Intereses: Ninguno relacionado a esta presentación. LBBB Stroke
 Las pesas se utilizan para realizar pesajes con balanzas mecánicas y más frecuentemente para el ajuste y la comprobación de balanzas electrónicas. La Organización Internacional de Metrología Legal (OIML)
Las pesas se utilizan para realizar pesajes con balanzas mecánicas y más frecuentemente para el ajuste y la comprobación de balanzas electrónicas. La Organización Internacional de Metrología Legal (OIML)
LAC-2009-09 Modificación 2.3.3.3. DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs
 LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs Current Policy 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this type of allocation
LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs Current Policy 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this type of allocation
Dr. Orlando Landrove. Jefe del Programa Nacional de ECNT. Minsap, Cuba
 Paho Project for Latinamerican Region Costa Rica, Cuba, Chile and México Dr. Orlando Landrove. Jefe del Programa Nacional de ECNT. Minsap, Cuba Que es el curso de diabetes on line? Iniciativa de OPS en
Paho Project for Latinamerican Region Costa Rica, Cuba, Chile and México Dr. Orlando Landrove. Jefe del Programa Nacional de ECNT. Minsap, Cuba Que es el curso de diabetes on line? Iniciativa de OPS en
Cirugía radical de próstata?
 ESP DECIPHER HABILITA A UN TRATAMIENTO PERSONALIZADO Y PROCESABLE DESPUÉS DE LA CIRUGÍA Cirugía radical de próstata? El Clasificador de Cáncer de Próstata Decipher puede ayudarlos a usted y a su médico
ESP DECIPHER HABILITA A UN TRATAMIENTO PERSONALIZADO Y PROCESABLE DESPUÉS DE LA CIRUGÍA Cirugía radical de próstata? El Clasificador de Cáncer de Próstata Decipher puede ayudarlos a usted y a su médico
Examen prenatal: Evaluación integrada En la Clínica de Medicina Materno Fetal en Yakima
 UW MEDICINE PATIENT EDUCATION PRENATAL TESTING: INTEGRATED SCREEN SPANISH Examen prenatal: Evaluación integrada En la Clínica de Medicina Materno Fetal en Yakima En la Clínica de Medicina Materno Fetal
UW MEDICINE PATIENT EDUCATION PRENATAL TESTING: INTEGRATED SCREEN SPANISH Examen prenatal: Evaluación integrada En la Clínica de Medicina Materno Fetal en Yakima En la Clínica de Medicina Materno Fetal
Advances and Trends in Chilean Boards
 Advances and Trends in Chilean Boards Dieter Linneberg A. Executive Director Centro de Gobierno Corporativo y Mercado de Capitales Universidad de Chile Context A study conducted by the center of corporate
Advances and Trends in Chilean Boards Dieter Linneberg A. Executive Director Centro de Gobierno Corporativo y Mercado de Capitales Universidad de Chile Context A study conducted by the center of corporate
TIPO DE CAMBIO AL CIERRE DE 2011 2 de enero de 2012 CLOSING EXCHANGE RATES AT YEAR END 2011 January 2, 2012. January 2, 2012 2 de enero de 2012
 CLOSING EXCHANGE RATES AT YEAR END 2011 TIPOS DE CAMBIO AL CIERRE DE 2011 January 2, 2012 2 de enero de 2012 This document is prepared by Acus Consulting and Alberto Calva. This document is available at
CLOSING EXCHANGE RATES AT YEAR END 2011 TIPOS DE CAMBIO AL CIERRE DE 2011 January 2, 2012 2 de enero de 2012 This document is prepared by Acus Consulting and Alberto Calva. This document is available at
PMI: Risk Management Certification Training (RMP)
 PMI: Risk Management Certification Training (RMP) Risk Management Certification Training (RMP) DESCRIPCIÓN: Este curso cubre las funciones y características de la Gestión de Riesgos para prepararse para
PMI: Risk Management Certification Training (RMP) Risk Management Certification Training (RMP) DESCRIPCIÓN: Este curso cubre las funciones y características de la Gestión de Riesgos para prepararse para
COMORBILIDADES en la HISTORIA CLINICA ELECTRONICA
 COMORBILIAES en la HISTORIA CLINICA ELECTRONICA r. RORIGUEZ, Jose Federico r. MARQUEZ FOSSER, Santiago Nicolas Charly Otero Hospital Italiano de Buenos Aires HCE + LISTA de PROBLEMAS HCE ORIENTAA a PROBLEMAS
COMORBILIAES en la HISTORIA CLINICA ELECTRONICA r. RORIGUEZ, Jose Federico r. MARQUEZ FOSSER, Santiago Nicolas Charly Otero Hospital Italiano de Buenos Aires HCE + LISTA de PROBLEMAS HCE ORIENTAA a PROBLEMAS
Tesis de Maestría titulada
 Tesis de Maestría titulada EL ANALISIS DE CONFIABILIDAD COMO HERRAMIENTA PARA OPTIMIZAR LA GESTIÓN DEL MANTENIMIENTO DE LOS EQUIPOS DE LA LÍNEA DE FLOTACIÓN EN UN CENTRO MINERO RESUMEN En la presente investigación
Tesis de Maestría titulada EL ANALISIS DE CONFIABILIDAD COMO HERRAMIENTA PARA OPTIMIZAR LA GESTIÓN DEL MANTENIMIENTO DE LOS EQUIPOS DE LA LÍNEA DE FLOTACIÓN EN UN CENTRO MINERO RESUMEN En la presente investigación
ESCUELA POLITECNICA NACIONAL INSTITUTO GEOFISICO
 IG-35 Quito, September 2, 25 Dr. Domenico Giardini FDSN Chair This letter is to express our official interest in joining the Federation of Digital Seismograph Networks (FDSN) and to present a brief description
IG-35 Quito, September 2, 25 Dr. Domenico Giardini FDSN Chair This letter is to express our official interest in joining the Federation of Digital Seismograph Networks (FDSN) and to present a brief description
1030 PATIENTS TREATED WITH MINIMALLY INVASIVE OZONE DISCOLYSIS IN LUMBAR DISC HERNIATION: 12 MONTHS FOLLOW-UP
 1030 PATIENTS TREATED WITH MINIMALLY INVASIVE OZONE DISCOLYSIS IN LUMBAR DISC HERNIATION: 12 MONTHS FOLLOW-UP Alejandro Ortiz-Basulto M.D. Cesar Alcantara-Canseco M.D. Eduardo Rivero-Sigarroa M.D. Jose
1030 PATIENTS TREATED WITH MINIMALLY INVASIVE OZONE DISCOLYSIS IN LUMBAR DISC HERNIATION: 12 MONTHS FOLLOW-UP Alejandro Ortiz-Basulto M.D. Cesar Alcantara-Canseco M.D. Eduardo Rivero-Sigarroa M.D. Jose
PEDRO SÁNCHEZ ROVIRA COMPLEJO HOSPITALARIO DE JAÉN
 PEDRO SÁNCHEZ ROVIRA COMPLEJO HOSPITALARIO DE JAÉN Maintenance therapy is the treatment of cancer with medication, typically following an initial round of treatment. Maintenance treatment may include chemotherapy,
PEDRO SÁNCHEZ ROVIRA COMPLEJO HOSPITALARIO DE JAÉN Maintenance therapy is the treatment of cancer with medication, typically following an initial round of treatment. Maintenance treatment may include chemotherapy,

 Full version is >>> HERE
Full version is >>> HERE