|
|
|
- Eva Bustos Villalobos
- hace 8 años
- Vistas:
Transcripción
1
2
3
4
5
6
7
8
9 Contents EDITORIAL International cooperation between vascular surgery programs to optimize education in the United States and Latin America: the time is right Luis R. Leon Jr. - Miguel F. Montero-Baker 11 ORIGINALS High Flow Iatrogenic Arteriovenous Fistula after Brachial Artery Puncture for Iliac Intervention Xiaoyi Teng, MD, Mireille A Moise, MD, Lisa Mican, et al. 15 Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. Ortiz, I.; Llasat N1. Riambau, V. 19 Intraoperatory Conic Beam Tomography (O-ARMTM) and Navigation assistance to Percutaneous Transgluteal Type II endoleak embolization: clinical and technical report. NJ. Mosquera, J. Castro. 24 Uterine arterio-venous malformation combined with aortic coarctation in a pregnant lady. Endovascular therapy and histerectomy. Case Report and literatura review. Dr. Jesús García Pérez, Dr. Jorge Arellano Sotelo, et al. 31 Pseudoaneurisma de arteria peronea asociado a fistula arteriovenosa: Tratamiento endovascular Dr. Diego López García 44 CONGRESS CALENDARY 48 The information and opinions expressed in the articles are exclusively those of the authors who are solely responsible of their contents. Técnicas Endovasculares is edited 3 times a year. Copyright NEWS FROM THE INDUSTRY INSTRUCTIONS FOR THE AUTOR No part of the articles of this publication may be reproduced without the prior written permission of the editor. SUBSCRIPTION FORM 09 62
10
11 Luis R Leon Jr. Miguel F Montero-Baker Editorial Dr. Luis R. Leon Jr. Dr. Miguel F. Montero-Baker 11
12 Luis R Leon Jr. Miguel F Montero-Baker Editorial A sad reality of most Latin American developing countries is caused the model by which most US-based endovascular companies have attempted to engage the market: the distributorship model. This complex model acts as a safety-net for large companies, since the local distributor assumes most of the risk involved in developing the business in uncharted seas; the unfortunate repercussion is the resulting ridiculous product overpricing (i.e. a angioplasty balloon in the US may cost $US 200, whereas in an emerging market the same product may be as high as $US 1,500). Due to the latter, vascular surgical interventions remain by large, open complex interventions, which, in many occasions, are what patients need, but in many other instances, these open interventions prove to be too invasive for patients that are often frail and in very poor medical condition. Patients then, if financially able, are tasked with finding a practitioner abroad that is capable and willing to perform the endovascular procedure needed, with ensuing multiple financial and logistic hurdles to overcome. Or the practitioner is asked to travel to a Latin country to perform this intervention, which is often complicated by similar financial and logistic hurdles, but also fails to overcome the availability restriction of certain endovascular tools to perform these procedures. This is an important component of the ever growing, unsupervised and non-regulated medical tourism. In the US, costs are less of a problem in terms of our ability to obtain medical devices such stents, balloons or catheters. In fact, this country has experienced a technological explosion during the last years, currently performing most vascular interventions through minimally invasive techniques. In a typical vascular practice, it is not uncommon to hear that a practitioner performs over 80% of his/her entire caseload through endovascular, minimally invasive methods. In our practice, the only areas in vascular surgery still dominated by open interventions are carotid and hemodialysis access interventions. Such a practice requires the use of devices and tools that are often quite expensive. Our restrictions are more set by the Food and Drug Administration and the speed at which new devices and technologies are approved for use in this country. Far from being an ideal situation, this has also caused tremendous implications for surgical training. The number of open cases that are performed nowadays in the US has dramatically dropped to alarming levels, making surgical training in standard procedures such as an open repair of an abdominal aortic aneurysm or a femoropedal arterial bypass a rare event. In current vascular practice, there is a real and strong need for proficiency with open procedures. Endovascular interventions have not completely replaced open procedures, and in my opinion we are far from this hypothetical situation. Therefore, graduates from current surgical training programs are in a disadvantageous position when joining established surgical practices. 12
13 Luis R Leon Jr. Miguel F Montero-Baker Editorial This discrepancy in access to resources has enormous implications on vascular surgery training, while creating an evident need for advanced training in peripheral interventions and vascular surgery education in Latin American countries. A surgeon is ultimately the sum of his or her cumulative operative experience, whether as the operating surgeon or assistant surgeon. Therefore it is imperative to utilize any possible opportunity to maximize this experience. Several alternatives for a solution have been sought. For instance, conducting surgical tutorials via videoconferencing or telemedicine undertaking at remote hospitals has been suggested, with positive results. For surgeons however, the hands-on experience is irreplaceable. We herein propose to incorporate away rotations overseas, in an exchange fashion between trainees in the US and those in Latin countries, for a number of months in order to improve the experience of US trainees in open vascular procedures and the endovascular experience of physicians overseas. As vascular practitioners in the US of Latino origin, our mission must be to take our strength in education and knowledge to those in need internationally. Guided by the belief that unnecessary amputations increase mortality and have a drastic negative economic impact, proper education and training will greatly improve the lives of the patients, their families and the communities in which they live. This could be accomplished by training and mentoring leading physicians and their team of healthcare providers. The ultimate goal is to create a network of physicians who can exchange ideas, new technologies and rely on each other as resource for vascular care. There are several examples of similar educational vascular surgical programs between the US and foreign countries, such as for instance China, that have been recently instituted, with enormous success. We must direct our efforts to the implementation of similar exchange programs between our region and the US. This will require significant dedication of time and financial resources. Fortunately, the recent economic growth of several Latin American countries has attracted the attention of several vascular device companies, and they have expressed their interest in supporting our mission. We have contacted several industry company officers as well as vascular surgery opinion leaders in both the US and Latin America in order for this to happen, and the level of interest is quite high. We believe that this is a project that has an enormous potential to change vascular training and to impact positively the care of vascular patients worldwide. The potential positive effects on vascular surgery education and care are limitless. This process would test the trainee s individual resilience and ability to adapt to new 13
14 Luis R Leon Jr. Miguel F Montero-Baker Editorial and sometimes strange-seeming situations, which could prove to be a major determinant in whether the future surgeon would thrive in his or her place of employment. This could have the benefit of producing surgeons who can work comfortably in any setting. Their surgical volume experience will be for sure enriched. Several professional networks of vascular practitioners would be created, which would serve as a constant source of future consulting. Several caveats to our proposal could be cited. For instance, the negative effects of social displacement, insufficient means to assert operative skills and quality of overseas faculty, language barriers and/or the potentially unsafe situation of some places in Latin America. This must be balanced against the positive results cited above. Away rotations from main campuses within the US have been the mainstay of training in this country. Globalization mandates at least to explore this possibility in this time of uncertainty in vascular surgery training. Our position in the vascular map and the timing is ideal. This is an opportunity that we cannot let pass by. Luis R Leon Jr., 1-5 Miguel F Montero-Baker1-2, 4-5 University of Arizona Health Science Center, Tucson, Arizona 1 Vascular and Endovascular Surgery Section - Tucson Medical Center, Tucson, Arizona 2 Arizona College of Osteopathic Medicine, Midwestern University, Phoenix, Arizona 3 Pima Heart Physicians - Vascular and Endovascular Surgery Section 4 Pima Vascular PC 5 14
15 Xiaoyi Teng, MD, Mireille A Moise, MD, Lisa Mican, et al. Fistula arteriovenosa yatrogénica de alto flujo secundaria a una punción braquial para intervencionisoo ilíaco. ORIGINALES Fistula arteriovenosa yatrogénica de alto flujo secundaria a una punción braquial para intervencionisoo ilíaco. High Flow Iatrogenic Arteriovenous Fistula after Brachial Artery Puncture for Iliac Intervention Xiaoyi Teng, MD, a Mireille A Moise, MD, b Lisa Mican, RVT, a Javier A Alvarez- Tostado, MD a From the Department of Vascular Surgery, Marymount Hospital, Cleveland Clinic,a and the Department of Vascular Surgery, Metrohealth Medical Center.b Javier A Alvarez-Tostado, MD, Department of Vascular Surgery, Marymount Hospital, Heart and Vascular Institute, Cleveland Clinic McCracken Road Suite 351, Garfield Hts., Ohio Tel Fax alvarej3@ccf.org 15 Resumen La arteria humeral ha sido establecida como un buen acceso para numerosas intervenciones endovasculars periféricas. Las complicaciones relacionadas con el acceso percutáeno braquial and sido escasamente reportadas en la literature. Informamos de un caso clínico con la presencia de una gran fistula arteriovenosa secundaria al abordaje arterial para una intervención ilíaca endovascular. Abstract: The brachial artery has been established as an important access site for a number of peripheral endovascular interventions. Complications from brachial percutaneous accesses have been sparsely reported in the literature. In this report, we present a case of a large, high flow brachial arteriovenous fistula secondary to sheath access for endovascular iliac intervention. Introduction The brachial artery has been established as an important access site for a number of peripheral endovascular interventions, as well as coronary and neurological interventions. (1,2) It has given interventionalists increased capacity and flexibility in the treatment of complex vascular problems and inaccessible vasculature. Complications from brachial percutaneous accesses have, however, been sparsely reported in the literature. Here we present a case of a large, high flow arteriovenous fistula (AVF) formation following sheath placement for arterial access for thrombolysis and subsequent intervention. Case Report: A 63-year-old male with a past medical history significant for hyperlipidemia, severe hypertension and heavy tobacco use presented to our department
16 Xiaoyi Teng, MD, Mireille A Moise, MD, Lisa Mican, et al. Fistula arteriovenosa yatrogénica de alto flujo secundaria a una punción braquial para intervencionisoo ilíaco. ORIGINALES Figure 1. Arteriovenous fistula duplex showing large fistula with high flow. for follow up after endovascular intervention for the treatment of acute ischemia of his left lower extremity. Three years prior, the patient was successfully treated with catheter directed thrombolysis and subsequent percutaneous angioplasty with stent placement in the left common and external iliac arteries. Left brachial access was obtained during his initial thrombolysis, and a 6-French sheath was placed without complications, over the point of maximal pulsation one finger breadth above the antecubital crease. The patient underwent a total of 48 hours of thrombolysis followed by angioplasty and left common and external 16 iliac stent placement. The patient tolerated all procedures well during his hospitalization, and his initial post-operative follow up was uneventful. The patient presented for follow up again after two years without any specific complaints. At that time, a palpable thrill was felt slightly proximal to his left antecubital fossa over the initial brachial access puncture site. The patient had no pain, edema or symptoms of steal syndrome in the left upper extremity. Radial pulses were 2+ bilaterally without significant difference between the two extremities. He denied any symptoms suggestive of heart ischemia or
17 Xiaoyi Teng, MD, Mireille A Moise, MD, Lisa Mican, et al. Fistula arteriovenosa yatrogénica de alto flujo secundaria a una punción braquial para intervencionisoo ilíaco. ORIGINALES Duplex ultrasound of the left upper extremity was performed which revealed a large arteriovenous fistula between the brachial artery and one of the brachial veins. The fistula was located approximately 2cm proximal to the brachial artery bifurcation. Flow within the arteriovenous fistula was measured using duplex and estimated to be 1091ml/min. (Figure 1) As stated above; the patient did not have systemic or local symptoms related to this fistula. However, due to the high flow as well as the low probability of spontaneous resolution, surgical repair was planned. The patient underwent open repair of the fistula, and was found to have a large, well-formed arteriovenous fistula approximately 5mm in diameter and almost 10mm in length. The affected brachial vein was located medial and anterior to the brachial artery. After proximal and distal control of both vessels was gained, the fistula was clamped and transected. Both the artery and the vein were both primarily repaired with 6-0 Prolene. (Figure 2) Subsequent follow up have been unremarkable with no sequelae from the repair up to 21 months after his surgical procedure. Duplex ultrasound revealed successful repair with no evidence of complications. Discussion: Iatrogenic injuries including occlusion, thrombosis and pseudoaneurysm formation have all been reported in the past decade as the usage of the brachial artery as an access site for vascular interventions has increased. In the coronary literature, the local complications have been reported to be approximately 0.4-3%, (3,4) with thrombosis of the brachial artery as the most reported complication. These percentages increase in cases of larger sheath size (7%) or in patients with smaller vessel sizes such as women (1,2,3). One notable peri-operative risk factor for injury included increased sheath length of >10cm for interventions. (2) 17 Figure 2. Operative findings and surgical repair.
18 Xiaoyi Teng, MD, Mireille A Moise, MD, Lisa Mican, et al. Fistula arteriovenosa yatrogénica de alto flujo secundaria a una punción braquial para intervencionisoo ilíaco. ORIGINALES In review of current literature, the occurrence of iatrogenic AVF formation following brachial artery puncture seem to be rare. (2,5) Most iatrogenic AVF have been reported following lower extremity puncture sites, namely the femoral artery and vein. (6) Prospective studies within the cardiac literature where all patients underwent post-operative femoral artery duplex exams document the overall incidence of AVF formation was <1%. (7,8) Most arteriovenous fistulas (90%) were asymptomatic and resolved without a surgical procedure within the first few months following intervention. The 10% that did require operative repair was usually due to large size or symptomatology, including swelling of affected limb, or in extreme cases, heart failure. Risk factors for the development of arteriovenous fistula after lower extremity punctures have included female gender and hypertension. Perioperative anticoagulation has also been attributed to an intrinsic decreased ability to thrombose small AVFs in the acute setting. (4) In our particular case, the patient had a history of hypertension and underwent thrombolysis and perioperative anticoagulation. Although the size of the sheath used was not large, it remained in place for 48 hours, making it a lengthy intervention. Operative findings showed that the affected brachial vein was located medial and anterior to the brachial artery. This particular anatomy, along with previously mentioned factors, increased the patient s risk for the development of vascular injury. Ultrasound-guided access possibly would have helped us prevent this complication. The lack of symptoms of most arteriovenous fistulas following arterial puncture often leads to spontaneous thrombosis before a diagnosis can be made. This may account for the limited amount of documentation of this complication seen within the literature. In our patient, the lack of symptoms resulted in an almost two year delay in diagnosis and repair, even though the fistula was large with high volume flow. If occurrence of brachial AVF can be inferred from the femoral literature, then even in the asymptomatic patient, the physician should carry a reasonable level of suspicion for the possibility of brachial arteriovenous fistula formation after access, especially if there are notable risk factors. References : 1. Criado FJ, Wilson EP, Abul-Khoudoud O, et al. Brachial artery catheterization to facilitate endovascular grafting of abdominal aortic aneurysm: safety and rationale. J Vasc Surg 2000;32: Alvarez-Tostado JA, Moise MA, et al. The brachial artery: a critical access for endovascular procedures. J Vasc Surg. 2009;49: Armstrong PJ, Han DC, Baxter JA, et al. Complication rates of percutaneous brachial artery access in peripheral vascular angiography. Ann Vasc Surg 2003;17: Tonnessen, BH. Iatrogenic injury from vascular access and endovascular procedures. Perspectives in Vascular Surgery and Endovascular Therapy, 2011;23(2): Khoury M, Batra S, Berg R, et al. Influence of arterial access sites and interventional procedures on vascular complications after cardiac catheterizations. Am J Surg Sep;164(3): Lazarides, MK, Tsoupanos, SS, Georgopoulos, SE, et al. Incidence and patterns of iatrogenic arterial injuries. A decade's experience. Journal of Cardiovascular Surgery, 1998; 39: Perings SF, Kelm M, Jax T, Strauer BE. A prospective study on incidence and risk factors of arteriovenous fistulae following transfemoral cardiac catheterization. Int J Cardiol. 2003;88: Ohlow MA, Secknus MA, von Korn H, et al. Incidence and outcome of femoral vascular complications among 18,165 patients undergoing cardiac catheterisation. Int J Cardiol Jun 12;135(1):66-71.
19 Ortiz, I.; Llasat N1. Riambau, V. Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. ORIGINALES Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. Aortic pseudo-sarcoma: confounding clinical and morphological findings Aortic Tumor-like lesion: endovascular solution Ortiz, I.; Llasat N 1. Riambau, V. División de Cirugía Vascular. Instituto del Tórax. 1 Enfermera quirofanista. Hospital Clínico. Universidad de Barcelona. Resumen Se presenta el caso de una mujer de 63 años de edad, con síndrome constitucional grave, claudicación intermitente de ambas extremidades inferiores y ausencia de pulsos femorales. Los estudios de imagen revelaron la presencia de una masa intraluminal que ocasinaba ocupación del 70% de la luz del segmento viscereal aórtica. Con la sospecha de angiosarcoma se sometió a biopsia endovascular y a tratamiento paliativo con stent aórtico no cubierto. Abstract We report a 63 year-old lady, with anorexia-cachexia, and asthenia syndrome, intermittent claudication, and femoral pulseless. Medical imaging revealed an intraluminal mass that let to a 70% of aortic stenosis at the visceral level. Angio-sarcoma was suspected and an endovascular biopsy and a palliative treatment with a aortic bare stent was applied. 19 Reporte Mujer de 63 años, antecedentes de interés alérgica al níquel, intolerancia a las estatinas, ciclopegicos, Hipertensa de reciente evolución que ha precisado el uso de drogas, dislipidemia, Fumadora de 2 paquetes de cigarrillos al día, Epoc, enfisema moderado, refiere que durante el otoño, después de vacunación para gripe estacional, inicia con astenia, adinamia, pérdida de peso, acompañado en una ocasión con febrícula. Además de presentar dolor abdominal inespecífico, autolimitado, con sabor fétido en la boca, claudicación de extremidades inferiores. Se le realiza angio Tc, donde se observa imagen calcificada pediculada que ocupa la luz de la aorta en su cara posterior que ocluye más del 70% de la luz(fig. 1,2); PET no capta, además de neumatosis gástrica e intestinal, a la exploración no hay pulsos femorales palpables, ante la presentación de la clínica se sospecha de síndrome constitucional por oclusión aortica a descartar sarcoma vs aterotrombosis, se le propuso tratamiento quirúrgico, sin embargo no aceptó abordaje abierto,
20 Ortiz, I.; Llasat N1. Riambau, V. Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. ORIGINALES por lo que se programó intervención endovascular, por vía percutánea a través de acceso femoral izquierdo, se practicó biopsias con forceps miocárdicos de material que obstruía la luz de la aorta, se enviaron restos a estudio histopatológico, la angioplastia se hizo con Stent aórtico E XL (Jotec,Hechingen Germany),(fig.3,4), previa protección de ramas viscerales con balones de oclusión para evitar embolias, la arteriorrafia de la A.femoral fue con parche de colageno, por hallarse placa de ateroma que condicionaba una estenosis de más del 50% a su salida, durante el postoperatorio inmediato se exploran pulsos femorales, los cuales se encuentran palpables en ambas extremidades y tibiales posteriores, se normaliza tensión arterial inmediatamente, no precisando continuar con medicación hipotensora, sin molestias abdominales, tolera la dieta oral y deambula sin claudicación. Figura 1 y 2. Lesión ocupativa de aorta. 20 El reporte de examen anatomopatológico, describe fragmento de coloración blanquecina de 7 mm de diámetro máximo, en la tinción con hematoxilina-eosina, se observó tejido fibroso a-celular entremezclando calcificaciones y ocasionales células endoteliales periféricas. Reporte final trombo y áreas calcificadas.
21 Ortiz, I.; Llasat N1. Riambau, V. Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. ORIGINALES Fig. 3. angioplastia de aorta con stent E-XL. (Jotec,Hechingen Germany) Discusion Las neoplasias primarias de aorta comprometen de igual manera a la aorta torácica y a la abdominal. La mayoría son clasificadas como sarcomas, entre ellos se encuentran el sarcoma intimal de la aorta, el angiosarcoma y el sarcoma de partes blandas. Los tumores no sarcomatosos benignos son extremadamente raros y se presentan más frecuentemente en adultos jóvenes y a los niños, localizados principalmente sobre la adventicia. Los paragangliomas, forman parte del diagnostico diferencial con los tumores de pared aórtica. La mayoría de los sarcomas se originan en la íntima, manifestándose con síntomas de obstrucción vascular por estrechamiento de la luz aórtica o incluso más común con embolización aterotrombotica periférica. 1 Los síntomas del angiosarcoma primario de aorta, simulan a los de la enfermedad oclusiva aterosclerótica y el patrón radiomorfológico a menudo es inespecífico. 2 21
22 Ortiz, I.; Llasat N1. Riambau, V. Aortic athero-thrombotic formation that morphologically and clinically mimics an Aortic sarcoma. ORIGINALES Las neoplasias primarias de aorta no tienen predilección por determinado sexo y aparecen en la edad media de la vida; su tratamiento requiere la exéresis del segmento vascular comprometido y tienen, en general, un pobre pronóstico. 3 El síndrome consuntivo o constitucional se ha identificado en el Hospital Universitario de Gran Canaria Doctor Negrín, Las Palmas, España con una prevalencia (aproximadamente 20 %).se caracteriza por astenia, adinamia y la pérdida involuntaria de peso con etiología orgánica, funcional e idiopática. Los tumores son las principales causas orgánicas representan aproximadamente 25 % de las causas, siguen los trastornos gastrointestinales y por último, las múltiples enfermedades crónicas cuando llegan a situaciones de máximo deterioro. Entre las causas psicosociales está la depresión y la demencia, aunque por lo general se tienen poco en cuenta al momento de la evaluación clínica en un paciente con pérdida de peso involuntaria sin aparente causa orgánica. 4 Tratamos de compartir esta experiencia en donde el diagnostico organizado, no nos condujo a la patología mas frecuente, sino al diagnostico diferencial este último, nos sirve para hacer una correcta valoración de una enfermedad con respecto a otras parecidas. Como en el caso clínico expuesto se consideró como diagnostico diferencial la patología ateroesclerótica ya que los signos y síntomas manifiestos por la frecuencia de la enfermedad, nos obligaron a realizar estudios complementarios para descartar y al mismo tiempo confirmar el diagnostico. Conclusion. El diagnóstico clínico es un arte, y sigue siendo un reto intelectual importante además de ser origen de satisfacciones en nuestra vida profesional, es la tarea fundamental de los médicos y la base para el tratamiento adecuado. No es una tarea fácil, ya que se conforma con la práctica diaria, conocimientos y sobretodo experiencia clínica. References: 1.- Higgins R, Posner MC, Moosa HH y col: Mesenteric infarction secondary to tumor emboly from primary aortic sarcoma. Cancer 1991; 68: Secondary Procedures After Infrarenal Abdominal Aortic Aneurysms Endovascular Repair With Second-Generation Endografts Michel A. Bartoli, Benjamin Thevenin, Gabrielle Sarlon, Roch Giorgi, Jean Noël Albertini, Gilles Lerussi, Alain Branchereau, Pierre-Edouard Magnan Annals of Vascular Surgery,Volume 28, Pages 490.e1 490.e4, February Primary angiosarcoma of the abdominal aorta: multi-row computed Tomography, Leopold Winter, Jan Langrehr, Enrique Lopez Hänninen, abdominal imaging August 2010, Volume 35, pp Bilbao-Garay J, Barba R, Losa-García JE, Martín H, García-de Casasola G, Castilla V, González-Anglada I, et al. Assessing clinical probability of organic disease in patients with involuntary weight loss: a simple score. Eur J Intern Med. 2002;13(4):
23 23
24 NJ. Mosquera, J. Castro, Intraoperatory Conic Beam Tomography (O-ARMTM) and Navigation assistance to Percutaneous Transgluteal Type II endoleak embolization: clinical and technical report. ORIGINALES Intraoperatory Conic Beam Tomography (O-ARMTM) and Navigation assistance to Percutaneous Transgluteal Type II endoleak embolization: clinical and technical report. NJ. Mosquera, 1 J. Castro, 2 1 Angiology and Vascular Surgery Department. Complexo Hospitalario Universitario de Ourense. Ourense. Spain. 2 Neurosurgery Department. Complexo Hospitalario Universitario de Ourense. Ourense. Spain. Corresponding author: NJ. Mosquera, Angiology and Vascular Surgery Department, Complexo Hospitalario Universitario de Ourense, 52-54, Ramon Puga St, 32005, Ourense, Spain. nmarochena@me.com Abstract Image guided surgery is a general description that can be applied to any surgical procedure, referenced by images, associated with specific surgical navigation devices. There has beeen a huge development of navigation systems to guide neurosurgical procedures. This technology can also be used to assist certain endovascular procedures such as the percutaneous translumbar / transgluteal embolization we are reporting. Case report: a type II endoleak with sac diameter enlargement related to patent hypogastric and gluteal artery and no direct access options was treated with a novel intraoperative image system 24 guidance, the Conic Beam Tomography (O-ARM), to acquire preoperative study combined with Navigation system and to guide the percutaneous transgluteal retrograde puncture of this artery. After the access was granted, we performed a coil embolization of the endoleak nidus plus Onyx TM embolization of hypogastric trunk. Successfull embolization and exclusion of the endoleak and hypogastric trunk was achieved with no intra or perioperative complications. The patient was discharged 18h later with no other complication. The procedure length was 55 minutes and the retrograde access puncture, guided by navigation, was achieved at first attemp.
25 NJ. Mosquera, J. Castro, Intraoperatory Conic Beam Tomography (O-ARMTM) and Navigation assistance to Percutaneous Transgluteal Type II endoleak embolization: clinical and technical report. ORIGINALES Discusion and Conclusions: The combination of Conic Beam Intraoperative Technology and Navigation system, as we are reporting, seems to be a promising approach to direct access to aneurysm sac when a translumbar embolization is needed. This was an easy, safe and fast procedure to solve a concerning complication related to EVAR. The accuracy of this approach is great as we demonstrated with the gluteal artery puncture. Key words: EVAR, embolization, endoleak, aneurysm, navigation Introduction Image guided surgery (IGS) is a developed concept wich includes any surgical procedure, performed under image assistance, with specifically designed medical devices, combined with anatomical images obtained previously or during the procedure. IGS, when is related to Neurosurgery, is usually designed Neuronavigation or just intraoperative navigation. These navigated procedures require specific medical devices (Navigators) which provide three dimensional orientation during the procedure, based on a previous computed tomography scan(ct), magnetic resonance image (MRI) or any other available image study accurate enough to give the system the proper anatomical references of the patient 1-3. Surgical Navigation step by step. 1. Image gathering: the most usual medical image study is CT or MRI performed previously to the procedure. These images can be fused with other image studies such as PET, SPECT, etc. 2. Image transfer process from regular source (usually Hospital PACS) to a computer or Navigator. 3. Matching technique; compare previous images with patient position on the operation table. Those images must be referenced with the actual position of the patient. There are different possible techniques to obtain an optimal match between image study and real anatomy of the patient: stickers with references applied to skin; bone reference, attached to patient percuteneously (screwed to patient s bone) or facial recognition as used in craneal surgery. These references will be identified by the navigator by optical (LEDs) or magnetic sensors. 4. Proper IGS: using different surgical devices, also with references the navigator is 25 capable to identify, the previous image study, actual patient s anatomy and surgical instruments are integrated by the navigator, displaying a virtual reconstruction of the surgical device position and its relation with actual anatomy. This system produces a virtual image, this image will guide the surgical procedure. Navigation systems are widely used in Neurosurgery for spine and craneal diseases such as tumors. These disesase have two common features; they are usually deeply located in high sensible áreas, where accuracy is critical, and they are also located in relativelly fix position in terms of anatomy. When craneal surgery is going to be performed, navigation references are glued to scalp. A facial anatomy recognition technique can be used also for the same aim. When Spine surgery is going to be performed, references will be fixed to the bone itself. This particular condition, the reference process, wich is completely neccesary to perform IGS, has been a limitation in the development of this technique to guide other surgical procedures such as Vascular or Endovascular procedures 4. O-ARM system & Stealth Station Treon Plus The O-ARM TM System (Medtronic, Minneapolis, US.) is an
Este proyecto tiene como finalidad la creación de una aplicación para la gestión y explotación de los teléfonos de los empleados de una gran compañía.
 SISTEMA DE GESTIÓN DE MÓVILES Autor: Holgado Oca, Luis Miguel. Director: Mañueco, MªLuisa. Entidad Colaboradora: Eli & Lilly Company. RESUMEN DEL PROYECTO Este proyecto tiene como finalidad la creación
SISTEMA DE GESTIÓN DE MÓVILES Autor: Holgado Oca, Luis Miguel. Director: Mañueco, MªLuisa. Entidad Colaboradora: Eli & Lilly Company. RESUMEN DEL PROYECTO Este proyecto tiene como finalidad la creación
MICINN Imágenes Médicas Publicaciones 2011-2012
 MICINN Imágenes Médicas Publicaciones 2011-2012 Iván Macía 11/01/2012 PUBLICACION 1 Macía, I.; Graña, M.; Maiora, J.; Paloc, C. & de Blas, M. Detection of type II endoleaks in abdominal aortic aneurysms
MICINN Imágenes Médicas Publicaciones 2011-2012 Iván Macía 11/01/2012 PUBLICACION 1 Macía, I.; Graña, M.; Maiora, J.; Paloc, C. & de Blas, M. Detection of type II endoleaks in abdominal aortic aneurysms
ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES
 ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES OXALIFE IMPLANTS SURFACE IN SMOKING AND NO SMOKING PATIENTS: A CLINICAL STUDY Autor: Malbos Marisel Director: Ibáñez
ESTUDIO CLÍNICO CON IMPLANTES DE SUPERFICIE OXALIFE EN PACIENTES FUMADORES Y NO FUMADORES OXALIFE IMPLANTS SURFACE IN SMOKING AND NO SMOKING PATIENTS: A CLINICAL STUDY Autor: Malbos Marisel Director: Ibáñez
Título del Proyecto: Sistema Web de gestión de facturas electrónicas.
 Resumen Título del Proyecto: Sistema Web de gestión de facturas electrónicas. Autor: Jose Luis Saenz Soria. Director: Manuel Rojas Guerrero. Resumen En la última década se han producido muchos avances
Resumen Título del Proyecto: Sistema Web de gestión de facturas electrónicas. Autor: Jose Luis Saenz Soria. Director: Manuel Rojas Guerrero. Resumen En la última década se han producido muchos avances
Volatilidad: Noviembre 2010 Futuros Frijol de Soya
 Observaciones Junio 09, 2010 1. La volatilidad tiene una tendencia a aumentar de Junio a Julio. 2. Este reporte sugiere que se debería considerar la implementación de estrategias largas con opciones en
Observaciones Junio 09, 2010 1. La volatilidad tiene una tendencia a aumentar de Junio a Julio. 2. Este reporte sugiere que se debería considerar la implementación de estrategias largas con opciones en
Sistemas de impresión y tamaños mínimos Printing Systems and minimum sizes
 Sistemas de impresión y tamaños mínimos Printing Systems and minimum sizes Para la reproducción del Logotipo, deberán seguirse los lineamientos que se presentan a continuación y que servirán como guía
Sistemas de impresión y tamaños mínimos Printing Systems and minimum sizes Para la reproducción del Logotipo, deberán seguirse los lineamientos que se presentan a continuación y que servirán como guía
TSQM (Version 1.4) Treatment Satisfaction Questionnaire for Medication
 TSQM (Version 1.4) Treatment Satisfaction Questionnaire for Medication Instructions: Please take some time to think about your level of satisfaction or dissatisfaction with the medication you are taking
TSQM (Version 1.4) Treatment Satisfaction Questionnaire for Medication Instructions: Please take some time to think about your level of satisfaction or dissatisfaction with the medication you are taking
ESCUELA POLITECNICA NACIONAL INSTITUTO GEOFISICO
 IG-35 Quito, September 2, 25 Dr. Domenico Giardini FDSN Chair This letter is to express our official interest in joining the Federation of Digital Seismograph Networks (FDSN) and to present a brief description
IG-35 Quito, September 2, 25 Dr. Domenico Giardini FDSN Chair This letter is to express our official interest in joining the Federation of Digital Seismograph Networks (FDSN) and to present a brief description
MANUAL EASYCHAIR. A) Ingresar su nombre de usuario y password, si ya tiene una cuenta registrada Ó
 MANUAL EASYCHAIR La URL para enviar su propuesta a la convocatoria es: https://easychair.org/conferences/?conf=genconciencia2015 Donde aparece la siguiente pantalla: Se encuentran dos opciones: A) Ingresar
MANUAL EASYCHAIR La URL para enviar su propuesta a la convocatoria es: https://easychair.org/conferences/?conf=genconciencia2015 Donde aparece la siguiente pantalla: Se encuentran dos opciones: A) Ingresar
http://mvision.madrid.org
 Apoyando el desarrollo de carrera de investigadores en imagen biomédica Supporting career development of researchers in biomedical imaging QUÉ ES M+VISION? WHAT IS M+VISION? M+VISION es un programa creado
Apoyando el desarrollo de carrera de investigadores en imagen biomédica Supporting career development of researchers in biomedical imaging QUÉ ES M+VISION? WHAT IS M+VISION? M+VISION es un programa creado
Why us? Porqué nosotros? URGENT REPORTS 12 HRS
 Rad-One Sotogrande Welcome to Rad-One Sotogrande. It is a privately owned independent radiology clinic located in the exclusive Puerto Deportivo Sotogrande. It is equipped with the latest high resolution
Rad-One Sotogrande Welcome to Rad-One Sotogrande. It is a privately owned independent radiology clinic located in the exclusive Puerto Deportivo Sotogrande. It is equipped with the latest high resolution
Aneurisma de Aorta abdominal
 Aneurisma de Aorta abdominal Tratamiento actual Dra. Caridi Maria de los Angeles Ateneo IDIM 09/Noviembre/2011 Aneurisma Dilatación permanente y localizada de una arteria que tiene, al menos, el 50 % de
Aneurisma de Aorta abdominal Tratamiento actual Dra. Caridi Maria de los Angeles Ateneo IDIM 09/Noviembre/2011 Aneurisma Dilatación permanente y localizada de una arteria que tiene, al menos, el 50 % de
Thank you. US English US Spanish. Australia-English Canada-English Ireland-English New Zealand-English Taiwan-English United Kingdom-English
 Dear Healthcare Provider, Included in this PDF are recruitment brochures in several languages to be used in MM Bone study (Protocol No.: 20090482). Kindly note these brochures have been updated according
Dear Healthcare Provider, Included in this PDF are recruitment brochures in several languages to be used in MM Bone study (Protocol No.: 20090482). Kindly note these brochures have been updated according
Contents. Introduction. Aims. Software architecture. Tools. Example
 ED@CON Control Results Management Software Control with Remote Sensing Contents Introduction Aims Software architecture Tools Example Introduction Control results management software (Ed@con) is a computer
ED@CON Control Results Management Software Control with Remote Sensing Contents Introduction Aims Software architecture Tools Example Introduction Control results management software (Ed@con) is a computer
Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo
 The American College of Obstetricians and Gynecologists WOMEN S HEALTH CARE PHYSICIANS Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo NOTA: Esta es una traducción libre realizada con la
The American College of Obstetricians and Gynecologists WOMEN S HEALTH CARE PHYSICIANS Traducido por: Dr. Pedro A. Vargas Torres Obstetra Ginecólogo NOTA: Esta es una traducción libre realizada con la
RESULTADOS DE COLOCACIÓN POR SECTOR PRODUCTIVO
 RESULTADOS DE COLOCACIÓN POR SECTOR PRODUCTIVO PLACEMENT RESULTS BY PRODUCTION SECTOR En este capítulo se presentarán los resultados de colocación que se realizaron a través de y de los fondos que éste
RESULTADOS DE COLOCACIÓN POR SECTOR PRODUCTIVO PLACEMENT RESULTS BY PRODUCTION SECTOR En este capítulo se presentarán los resultados de colocación que se realizaron a través de y de los fondos que éste
SIGUIENDO LOS REQUISITOS ESTABLECIDOS EN LA NORMA ISO 14001 Y CONOCIENDO LAS CARACTERISTICAS DE LA EMPRESA CARTONAJES MIGUEL Y MATEO EL ALUMNO DEBERA
 SIGUIENDO LOS REQUISITOS ESTABLECIDOS EN LA NORMA ISO 14001 Y CONOCIENDO LAS CARACTERISTICAS DE LA EMPRESA CARTONAJES MIGUEL Y MATEO EL ALUMNO DEBERA ELABORAR LA POLITICA AMBIENTAL PDF File: Siguiendo
SIGUIENDO LOS REQUISITOS ESTABLECIDOS EN LA NORMA ISO 14001 Y CONOCIENDO LAS CARACTERISTICAS DE LA EMPRESA CARTONAJES MIGUEL Y MATEO EL ALUMNO DEBERA ELABORAR LA POLITICA AMBIENTAL PDF File: Siguiendo
From e-pedagogies to activity planners. How can it help a teacher?
 From e-pedagogies to activity planners. How can it help a teacher? Elena de Miguel, Covadonga López, Ana Fernández-Pampillón & Maria Matesanz Universidad Complutense de Madrid ABSTRACT Within the framework
From e-pedagogies to activity planners. How can it help a teacher? Elena de Miguel, Covadonga López, Ana Fernández-Pampillón & Maria Matesanz Universidad Complutense de Madrid ABSTRACT Within the framework
QUE ES EL CANCER DE MAMA PDF
 QUE ES EL CANCER DE MAMA PDF ==> Download: QUE ES EL CANCER DE MAMA PDF QUE ES EL CANCER DE MAMA PDF - Are you searching for Que Es El Cancer De Mama Books? Now, you will be happy that at this time Que
QUE ES EL CANCER DE MAMA PDF ==> Download: QUE ES EL CANCER DE MAMA PDF QUE ES EL CANCER DE MAMA PDF - Are you searching for Que Es El Cancer De Mama Books? Now, you will be happy that at this time Que
Agustiniano Ciudad Salitre School Computer Science Support Guide - 2015 Second grade First term
 Agustiniano Ciudad Salitre School Computer Science Support Guide - 2015 Second grade First term UNIDAD TEMATICA: INTERFAZ DE WINDOWS LOGRO: Reconoce la interfaz de Windows para ubicar y acceder a los programas,
Agustiniano Ciudad Salitre School Computer Science Support Guide - 2015 Second grade First term UNIDAD TEMATICA: INTERFAZ DE WINDOWS LOGRO: Reconoce la interfaz de Windows para ubicar y acceder a los programas,
ADAPTACIÓN DE REAL TIME WORKSHOP AL SISTEMA OPERATIVO LINUX
 ADAPTACIÓN DE REAL TIME WORKSHOP AL SISTEMA OPERATIVO LINUX Autor: Tomás Murillo, Fernando. Director: Muñoz Frías, José Daniel. Coordinador: Contreras Bárcena, David Entidad Colaboradora: ICAI Universidad
ADAPTACIÓN DE REAL TIME WORKSHOP AL SISTEMA OPERATIVO LINUX Autor: Tomás Murillo, Fernando. Director: Muñoz Frías, José Daniel. Coordinador: Contreras Bárcena, David Entidad Colaboradora: ICAI Universidad
Universidad de Guadalajara
 Universidad de Guadalajara Centro Universitario de Ciencias Económico-Administrativas Maestría en Tecnologías de Información Ante-proyecto de Tésis Selection of a lightweight virtualization framework to
Universidad de Guadalajara Centro Universitario de Ciencias Económico-Administrativas Maestría en Tecnologías de Información Ante-proyecto de Tésis Selection of a lightweight virtualization framework to
QUE ES CANCER DE MAMA PDF
 QUE ES CANCER DE MAMA PDF ==> Download: QUE ES CANCER DE MAMA PDF QUE ES CANCER DE MAMA PDF - Are you searching for Que Es Cancer De Mama Books? Now, you will be happy that at this time Que Es Cancer De
QUE ES CANCER DE MAMA PDF ==> Download: QUE ES CANCER DE MAMA PDF QUE ES CANCER DE MAMA PDF - Are you searching for Que Es Cancer De Mama Books? Now, you will be happy that at this time Que Es Cancer De
TITLE VI COMPLAINT FORM
 [CITY SEAL/EMBLEM] The Capital City of the Palm Beaches TITLE VI COMPLAINT FORM Title VI of the 1964 Civil Rights Act requires that "No person in the United States shall, on the ground of race, color or
[CITY SEAL/EMBLEM] The Capital City of the Palm Beaches TITLE VI COMPLAINT FORM Title VI of the 1964 Civil Rights Act requires that "No person in the United States shall, on the ground of race, color or
SISTEMA DE GESTIÓN Y ANÁLISIS DE PUBLICIDAD EN TELEVISIÓN
 SISTEMA DE GESTIÓN Y ANÁLISIS DE PUBLICIDAD EN TELEVISIÓN Autor: Barral Bello, Alfredo Director: Alcalde Lancharro, Eduardo Entidad Colaboradora: Media Value S.L. RESUMEN DEL PROYECTO El presente proyecto
SISTEMA DE GESTIÓN Y ANÁLISIS DE PUBLICIDAD EN TELEVISIÓN Autor: Barral Bello, Alfredo Director: Alcalde Lancharro, Eduardo Entidad Colaboradora: Media Value S.L. RESUMEN DEL PROYECTO El presente proyecto
SEGUIMIENTO A MEDIANO PLAZO CON ENDOPROTESIS SETA, BALÓN EXPANDIBLE PARA EL TRATAMIENTO DEL ANEURISMA DE AORTA ABDOMINAL
 SEGUIMIENTO A MEDIANO PLAZO CON ENDOPROTESIS SETA, BALÓN EXPANDIBLE PARA EL TRATAMIENTO DEL ANEURISMA DE AORTA ABDOMINAL Dr. Girela Alejandro German Instituto Cardiovascular del Sur, Cipolletti, Rio Negro
SEGUIMIENTO A MEDIANO PLAZO CON ENDOPROTESIS SETA, BALÓN EXPANDIBLE PARA EL TRATAMIENTO DEL ANEURISMA DE AORTA ABDOMINAL Dr. Girela Alejandro German Instituto Cardiovascular del Sur, Cipolletti, Rio Negro
Sistema!de!iluminación!de!un!longboard!
 Sistemadeiluminacióndeunlongboard RESUMEN JuanJacoboMonteroMuñoz GradoenIngenieríaelectromecánica,electrónicaindustrial DoblediplomaconSupélecParís. Este proyecto ha sido desarrollado en París, en la Ecole
Sistemadeiluminacióndeunlongboard RESUMEN JuanJacoboMonteroMuñoz GradoenIngenieríaelectromecánica,electrónicaindustrial DoblediplomaconSupélecParís. Este proyecto ha sido desarrollado en París, en la Ecole
RDA in BNE. Mar Hernández Agustí Technical Process Department Manager Biblioteca Nacional de España
 RDA in BNE Mar Hernández Agustí Technical Process Department Manager Biblioteca Nacional de España RDA at the National Library of Spain: BNE preparation for new Cataloguing Rules Since 2007 BNE has been
RDA in BNE Mar Hernández Agustí Technical Process Department Manager Biblioteca Nacional de España RDA at the National Library of Spain: BNE preparation for new Cataloguing Rules Since 2007 BNE has been
LAC-2009-09 Modificación 2.3.3.3. DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs
 LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs Current Policy 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this type of allocation
LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES INICIALES A ISPs Current Policy 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this type of allocation
TEXAS DEPARTMENT OF STATE HEALTH SERVICES
 TEXAS DEPARTMENT OF STATE HEALTH SERVICES DAVID L. LAKEY, M.D. COMMISSIONER P.O. Box 149347 Austin, Texas 78714-9347 1-888-963-7111 TTY: 1-800-735-2989 www.dshs.state.tx.us August 15, 2013 Dear Birthing
TEXAS DEPARTMENT OF STATE HEALTH SERVICES DAVID L. LAKEY, M.D. COMMISSIONER P.O. Box 149347 Austin, Texas 78714-9347 1-888-963-7111 TTY: 1-800-735-2989 www.dshs.state.tx.us August 15, 2013 Dear Birthing
Types of Dementia. Common Causes of Dementia
 Types of Dementia Dementia is a loss of skills to think, remember and reason that is severe enough to affect daily activities. It is normal to need more time to remember things as we get older. Other thinking
Types of Dementia Dementia is a loss of skills to think, remember and reason that is severe enough to affect daily activities. It is normal to need more time to remember things as we get older. Other thinking
Creating your Single Sign-On Account for the PowerSchool Parent Portal
 Creating your Single Sign-On Account for the PowerSchool Parent Portal Welcome to the Parent Single Sign-On. What does that mean? Parent Single Sign-On offers a number of benefits, including access to
Creating your Single Sign-On Account for the PowerSchool Parent Portal Welcome to the Parent Single Sign-On. What does that mean? Parent Single Sign-On offers a number of benefits, including access to
Raíz aórtica dilatada y aorta ascendente asintomáticas: Qué podemos hacer? Pueden las guías guiarnos? Tirone E. David University of Toronto
 Raíz aórtica dilatada y aorta ascendente asintomáticas: Qué podemos hacer? Pueden las guías guiarnos? Tirone E. David University of Toronto Raíz aórtica dilatada y aorta ascendente asintomáticas: Qué podemos
Raíz aórtica dilatada y aorta ascendente asintomáticas: Qué podemos hacer? Pueden las guías guiarnos? Tirone E. David University of Toronto Raíz aórtica dilatada y aorta ascendente asintomáticas: Qué podemos
Final Project (academic investigation)
 Final Project (academic investigation) MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Final Project (academic
Final Project (academic investigation) MÁSTER UNIVERSITARIO EN BANCA Y FINANZAS (Finance & Banking) Universidad de Alcalá Curso Académico 2015/16 GUÍA DOCENTE Nombre de la asignatura: Final Project (academic
Tipo del póster: Presentación Electrónica Educativa Autores:
 Endofugas o Endoleaks en Prótesis Endovasculares de Aneurismas de Aorta Abdominal: Lo que el Radiólogo debe saber en relación al Diagnóstico, Caracterización y Principios Básicos de Manejo. Poster no.:
Endofugas o Endoleaks en Prótesis Endovasculares de Aneurismas de Aorta Abdominal: Lo que el Radiólogo debe saber en relación al Diagnóstico, Caracterización y Principios Básicos de Manejo. Poster no.:
DONACION DE OLD TIME FOUNDATION A NIKAO MAORI SCHOOL RAROTONGA ISLAS COOK OCTUBRE 2007
 DONACION DE OLD TIME FOUNDATION A NIKAO MAORI SCHOOL RAROTONGA ISLAS COOK OCTUBRE 2007 La escuela primaria Nikao Maori School fue fundada en 1955. Es una escuela pública y tiene actualmente 123 alumnos.
DONACION DE OLD TIME FOUNDATION A NIKAO MAORI SCHOOL RAROTONGA ISLAS COOK OCTUBRE 2007 La escuela primaria Nikao Maori School fue fundada en 1955. Es una escuela pública y tiene actualmente 123 alumnos.
Welcome to lesson 2 of the The Spanish Cat Home learning Spanish course.
 Welcome to lesson 2 of the The Spanish Cat Home learning Spanish course. Bienvenidos a la lección dos. The first part of this lesson consists in this audio lesson, and then we have some grammar for you
Welcome to lesson 2 of the The Spanish Cat Home learning Spanish course. Bienvenidos a la lección dos. The first part of this lesson consists in this audio lesson, and then we have some grammar for you
The 10 Building Blocks of Primary Care
 The 10 Building Blocks of Primary Care My Action Plan Background and Description The Action Plan is a tool used to engage patients in behavior-change discussion with a clinician or health coach. Using
The 10 Building Blocks of Primary Care My Action Plan Background and Description The Action Plan is a tool used to engage patients in behavior-change discussion with a clinician or health coach. Using
manual de servicio nissan murano z51
 manual de servicio nissan murano z51 Reference Manual To understand featuring to use and how to totally exploit manual de servicio nissan murano z51 to your great advantage, there are several sources of
manual de servicio nissan murano z51 Reference Manual To understand featuring to use and how to totally exploit manual de servicio nissan murano z51 to your great advantage, there are several sources of
What is family health history?
 Family Health History Project Pre-Survey What is family health history? Family health history is information about diseases that run in your family, as well as the eating habits, activities, and environments
Family Health History Project Pre-Survey What is family health history? Family health history is information about diseases that run in your family, as well as the eating habits, activities, and environments
English Literacy Success Team, e3 Civic High October 30, 2014
 English Literacy Success Team, e3 Civic High October 30, 2014 What is the English Language Success Team? The purpose of our committee is to provide an open conversation between parents, students, and teachers
English Literacy Success Team, e3 Civic High October 30, 2014 What is the English Language Success Team? The purpose of our committee is to provide an open conversation between parents, students, and teachers
UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR.
 UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR. Autor: Ruiz Muñoz, Rafael. Director: Muñoz García, Manuel. Entidad Colaboradora: Empresarios Agrupados.
UTILIZACIÓN DE UN BOLÍGRAFO DÍGITAL PARA LA MEJORA DE PROCEDIMIENTOS DE CAMPO EN UNA CENTRAL NUCLEAR. Autor: Ruiz Muñoz, Rafael. Director: Muñoz García, Manuel. Entidad Colaboradora: Empresarios Agrupados.
CIRUGIA MINIMAMENTE INVASORA EN EL MANEJO DEL TRAUMA ABDOMINAL CERRADO POR EXPLOSION UNA ALTERNATIVA? POR: DANIEL HERNANDO GARCIA VILLAMIZAR M.D.
 UNIVERSIDAD MILITAR NUEVA GRANADA FACULTAD DE MEDICINA CIRUGIA MINIMAMENTE INVASORA EN EL MANEJO DEL TRAUMA ABDOMINAL CERRADO POR EXPLOSION UNA ALTERNATIVA? POR: DANIEL HERNANDO GARCIA VILLAMIZAR M.D.
UNIVERSIDAD MILITAR NUEVA GRANADA FACULTAD DE MEDICINA CIRUGIA MINIMAMENTE INVASORA EN EL MANEJO DEL TRAUMA ABDOMINAL CERRADO POR EXPLOSION UNA ALTERNATIVA? POR: DANIEL HERNANDO GARCIA VILLAMIZAR M.D.
News Flash! Primary & Specialty Care Providers. Sharp Health Plan. Date: February 17, 2012. Subject: Member Grievance Forms
 I M P O R T A N T News Flash! A FAX Publication for Providers of Sharp Health Plan To: From: Primary & Specialty Care Providers Sharp Health Plan Date: February 17, 2012 Subject: Member Grievance Forms
I M P O R T A N T News Flash! A FAX Publication for Providers of Sharp Health Plan To: From: Primary & Specialty Care Providers Sharp Health Plan Date: February 17, 2012 Subject: Member Grievance Forms
Adobe Acrobat Reader X: Manual to Verify the Digital Certification of a Document
 dobe crobat Reader X: Manual de verificación de Certificación Digital de un documento dobe crobat Reader X: Manual to Verify the Digital Certification of a Document support@bioesign.com Desarrollado por:
dobe crobat Reader X: Manual de verificación de Certificación Digital de un documento dobe crobat Reader X: Manual to Verify the Digital Certification of a Document support@bioesign.com Desarrollado por:
Registro de Semilla y Material de Plantación
 Registro de Semilla y Material de Plantación Este registro es para documentar la semilla y material de plantación que usa, y su estatus. Mantenga las facturas y otra documentación pertinente con sus registros.
Registro de Semilla y Material de Plantación Este registro es para documentar la semilla y material de plantación que usa, y su estatus. Mantenga las facturas y otra documentación pertinente con sus registros.
Brain Tumors. Glioma Tumors
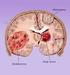 Brain Tumors A tumor that starts and grows in the brain is called a primary brain tumor. Primary brain tumors get their name from the type of cell or the part of the brain where they start growing. A secondary
Brain Tumors A tumor that starts and grows in the brain is called a primary brain tumor. Primary brain tumors get their name from the type of cell or the part of the brain where they start growing. A secondary
La Calidad como determinante de la demanda de servicios de atención médica primaria en México
 FACULTAD LATINOAMERICANA DE CIENCIAS SOCIALES SEDE ACADÉMICA DE MÉXICO Doctorado en Investigación en Ciencias sociales con mención en Ciencia Política VII (Séptima Promoción) 2008 2011 La Calidad como
FACULTAD LATINOAMERICANA DE CIENCIAS SOCIALES SEDE ACADÉMICA DE MÉXICO Doctorado en Investigación en Ciencias sociales con mención en Ciencia Política VII (Séptima Promoción) 2008 2011 La Calidad como
Edgar Quiñones. HHRR: Common Sense Does Not Mean Business. Objective
 Edgar Quiñones HHRR: Common Sense Does Not Mean Business Objective Share experiences & insight gained in the last two decades in the management consulting business regarding why Common Sense Does Not Mean
Edgar Quiñones HHRR: Common Sense Does Not Mean Business Objective Share experiences & insight gained in the last two decades in the management consulting business regarding why Common Sense Does Not Mean
PRINTING INSTRUCTIONS
 PRINTING INSTRUCTIONS 1. Print the Petition form on 8½ X 11inch paper. 2. The second page (instructions for circulator) must be copied on the reverse side of the petition Instructions to print the PDF
PRINTING INSTRUCTIONS 1. Print the Petition form on 8½ X 11inch paper. 2. The second page (instructions for circulator) must be copied on the reverse side of the petition Instructions to print the PDF
iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain)
 iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain) ! Introduction! Passage Retrieval Systems! IR-n system! IR-n system at iclef-2002! Conclusions and Future works ! Introduction!
iclef-2002 at Universities of Alicante and Jaen University of Alicante (Spain) ! Introduction! Passage Retrieval Systems! IR-n system! IR-n system at iclef-2002! Conclusions and Future works ! Introduction!
IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR
 IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR Subject: Important Updates Needed for Your FAFSA Dear [Applicant], When you completed your 2012-2013 Free Application for Federal Student Aid
IRS DATA RETRIEVAL NOTIFICATION DEPENDENT STUDENT ESTIMATOR Subject: Important Updates Needed for Your FAFSA Dear [Applicant], When you completed your 2012-2013 Free Application for Federal Student Aid
PROYECTO INFORMÁTICO PARA LA CREACIÓN DE UN GESTOR DOCUMENTAL PARA LA ONG ENTRECULTURAS
 PROYECTO INFORMÁTICO PARA LA CREACIÓN DE UN GESTOR DOCUMENTAL PARA LA ONG ENTRECULTURAS Autor: García Lodares, Victor. Director: Castejón Silvo, Pedro. Entidad Colaboradora: Entreculturas. Resumen del
PROYECTO INFORMÁTICO PARA LA CREACIÓN DE UN GESTOR DOCUMENTAL PARA LA ONG ENTRECULTURAS Autor: García Lodares, Victor. Director: Castejón Silvo, Pedro. Entidad Colaboradora: Entreculturas. Resumen del
EL ESTILO INDIRECTO (REPORTED SPEECH)
 EL ESTILO INDIRECTO () **El estilo indirecto es la forma de reproducir en tercera persona lo que alguien ha dicho textualmente. I m tired she said. She said that she was tired. Como se observa en el ejemplo
EL ESTILO INDIRECTO () **El estilo indirecto es la forma de reproducir en tercera persona lo que alguien ha dicho textualmente. I m tired she said. She said that she was tired. Como se observa en el ejemplo
The Home Language Survey (HLS) and Identification of Students
 The Home Language Survey (HLS) and Identification of Students The Home Language Survey (HLS) is the document used to determine a student that speaks a language other than English. Identification of a language
The Home Language Survey (HLS) and Identification of Students The Home Language Survey (HLS) is the document used to determine a student that speaks a language other than English. Identification of a language
La mortalidad inmediata total fue de 3,3%. La frecuencia de mortalidad para los grupos fue de 6,5% (n= 6) vs. 1,9% (n= 4) respectivamente.
 33 Bogotá, Colombia. Existen controversias acerca de las posibles ventajas del abordaje transperitoneal vs. extraperitoneal en la cirugía de aneurisma de aorta abdominal; con este último, algunos estudios
33 Bogotá, Colombia. Existen controversias acerca de las posibles ventajas del abordaje transperitoneal vs. extraperitoneal en la cirugía de aneurisma de aorta abdominal; con este último, algunos estudios
Instructor: She just said that she s Puerto Rican. Escucha y repite la palabra Puerto Rican -for a man-.
 Learning Spanish Like Crazy Spoken Spanish Lección once Instructor: Cómo se dice Good afternoon? René: Buenas tardes. Buenas tardes. Instructor: How do you ask a woman if she s Colombian. René: Eres Colombiana?
Learning Spanish Like Crazy Spoken Spanish Lección once Instructor: Cómo se dice Good afternoon? René: Buenas tardes. Buenas tardes. Instructor: How do you ask a woman if she s Colombian. René: Eres Colombiana?
Health in Peru, 1991-2003. Prepared by Leigh Campoamor
 Prepared by Leigh Campoamor Princeton University Library Princeton, NJ 2003 Scope Note Contents: This collection contains pamphlets, articles, and other miscellaneous items addressing a range of health-related
Prepared by Leigh Campoamor Princeton University Library Princeton, NJ 2003 Scope Note Contents: This collection contains pamphlets, articles, and other miscellaneous items addressing a range of health-related
EN United in diversity EN A8-0204/83. Amendment
 27.6.2018 A8-0204/83 83 Recital 2 (2) So far, and unless otherwise provided for in national law, the rules on access to the occupation of road transport operator do not apply to undertakings engaged in
27.6.2018 A8-0204/83 83 Recital 2 (2) So far, and unless otherwise provided for in national law, the rules on access to the occupation of road transport operator do not apply to undertakings engaged in
Puede pagar facturas y gastos periódicos como el alquiler, el gas, la electricidad, el agua y el teléfono y también otros gastos del hogar.
 SPANISH Centrepay Qué es Centrepay? Centrepay es la manera sencilla de pagar sus facturas y gastos. Centrepay es un servicio de pago de facturas voluntario y gratuito para clientes de Centrelink. Utilice
SPANISH Centrepay Qué es Centrepay? Centrepay es la manera sencilla de pagar sus facturas y gastos. Centrepay es un servicio de pago de facturas voluntario y gratuito para clientes de Centrelink. Utilice
DUAL IMMERSION PROGRAM INFORMATION PRESCHOOL PRESENTATION SEPTEMBER 10, 2014 6:30 P.M.
 DUAL IMMERSION PROGRAM INFORMATION PRESCHOOL PRESENTATION SEPTEMBER 10, 2014 6:30 P.M. Presented by Dr. Norma R. Delgado, Director of Curriculum & Instruction 1 The United States Government has identified
DUAL IMMERSION PROGRAM INFORMATION PRESCHOOL PRESENTATION SEPTEMBER 10, 2014 6:30 P.M. Presented by Dr. Norma R. Delgado, Director of Curriculum & Instruction 1 The United States Government has identified
Conditioning Exercises: Standing
 Conditioning Exercises: Standing Do all these exercises slowly. Do not hold your breath during these exercises. If unusual pain occurs in your joints or muscles while you are exercising, do not continue
Conditioning Exercises: Standing Do all these exercises slowly. Do not hold your breath during these exercises. If unusual pain occurs in your joints or muscles while you are exercising, do not continue
Gaia en las universidades españolas y los centros de inves3gación
 Gaia en las universidades españolas y los centros de inves3gación Ana Ulla Miguel (GGG) Depto. de Física Aplicada, Universidade de Vigo The GGG group is presently composed of the following members: Dra.
Gaia en las universidades españolas y los centros de inves3gación Ana Ulla Miguel (GGG) Depto. de Física Aplicada, Universidade de Vigo The GGG group is presently composed of the following members: Dra.
SELF ASSESSMENT TOOL: DRR CAPACITIES AT LOCAL LEVEL. Dominican Republic
 A quick resume SELF ASSESSMENT TOOL: DRR CAPACITIES AT LOCAL LEVEL Dominican Republic DIPECHO project Strengthening local capacities for response and management of risks with respect to seismic events
A quick resume SELF ASSESSMENT TOOL: DRR CAPACITIES AT LOCAL LEVEL Dominican Republic DIPECHO project Strengthening local capacities for response and management of risks with respect to seismic events
General Certificate of Education Advanced Level Examination June 2013
 General Certificate of Education Advanced Level Examination June 2013 Spanish Unit 4 Speaking Test Candidate s Material To be conducted by the teacher examiner between 7 March and 15 May 2013 (SPA4T) To
General Certificate of Education Advanced Level Examination June 2013 Spanish Unit 4 Speaking Test Candidate s Material To be conducted by the teacher examiner between 7 March and 15 May 2013 (SPA4T) To
Beneficios de Fundar una Corporación Sin Fines de Lucro Benefits of Establishing a Non-Profit Corporation
 ISSN 2152-6613 Beneficios de Fundar una Corporación Sin Fines de Lucro Benefits of Establishing a Non-Profit Corporation Evaluación Capacitación Rendimiento NPERCI Publication Series No. 2 Flordeliz Serpa,
ISSN 2152-6613 Beneficios de Fundar una Corporación Sin Fines de Lucro Benefits of Establishing a Non-Profit Corporation Evaluación Capacitación Rendimiento NPERCI Publication Series No. 2 Flordeliz Serpa,
OSH: Integrated from school to work.
 SST: Integrada desde la escuela hasta el empleo. OSH: Integrated from school to work. ESPAÑA - SPAIN Mª Mercedes Tejedor Aibar José Luis Castellá López Instituto Nacional de Seguridad e Higiene en el Trabajo
SST: Integrada desde la escuela hasta el empleo. OSH: Integrated from school to work. ESPAÑA - SPAIN Mª Mercedes Tejedor Aibar José Luis Castellá López Instituto Nacional de Seguridad e Higiene en el Trabajo
Sistema de Oclusión Nit-Occlud PDA Dispositivo-coil de nitinol coil para ductus de 2 a 4mm
 Sistema de Oclusión Nit-Occlud PDA Dispositivo-coil de nitinol coil para ductus de 2 a 4mm Dr. Frank Thiel, Marketing Manager 1 Product infomation PDA Soluciones con Nit-Occlud (PDA 2 a 4mm) Sistema premontado
Sistema de Oclusión Nit-Occlud PDA Dispositivo-coil de nitinol coil para ductus de 2 a 4mm Dr. Frank Thiel, Marketing Manager 1 Product infomation PDA Soluciones con Nit-Occlud (PDA 2 a 4mm) Sistema premontado
Presentación inusual de un hemangioma cavernoso de mama
 CASO CLÍNICO Anales de Radiología México Presentación inusual de un hemangioma cavernoso de mama RESUMEN Los hemangiomas son tumores benignos de origen vascular cuya pre publicaciones que describan sus
CASO CLÍNICO Anales de Radiología México Presentación inusual de un hemangioma cavernoso de mama RESUMEN Los hemangiomas son tumores benignos de origen vascular cuya pre publicaciones que describan sus
SPANISH ORAL LANGUAGE ASSESSMENT. Jill Jegerski Department of Modern Languages April 8, 2011
 SPANISH ORAL LANGUAGE ASSESSMENT Jill Jegerski Department of Modern Languages April 8, 2011 INTRODUCTION Basic Spanish program at CSI Three-course Gen. Ed. sequence: SPN 113, 114, 213 Approximately 800
SPANISH ORAL LANGUAGE ASSESSMENT Jill Jegerski Department of Modern Languages April 8, 2011 INTRODUCTION Basic Spanish program at CSI Three-course Gen. Ed. sequence: SPN 113, 114, 213 Approximately 800
Steps to Understand Your Child s Behavior. Customizing the Flyer
 Steps to Understand Your Child s Behavior Customizing the Flyer Hello! Here is the PDF Form Template for use in advertising Steps to Understanding Your Child s Behavior (HDS Behavior Level 1B). Because
Steps to Understand Your Child s Behavior Customizing the Flyer Hello! Here is the PDF Form Template for use in advertising Steps to Understanding Your Child s Behavior (HDS Behavior Level 1B). Because
Certificación en España según normas UNE-EN-ISO 9000 y 14000
 Certificación en España según normas UNE-EN-ISO 9000 y 14000 Sexto informe de Forum Calidad Es este el sexto informe que Forum Calidad presenta sobre el número y distribución de las organizaciones españolas
Certificación en España según normas UNE-EN-ISO 9000 y 14000 Sexto informe de Forum Calidad Es este el sexto informe que Forum Calidad presenta sobre el número y distribución de las organizaciones españolas
Solicitud de Intercambio Academico por Convenio Bilateral UPAEP para alumnos extranjeros
 Solicitud de Intercambio Academico por Convenio Bilateral UPAEP para alumnos extranjeros INFORMACION PERSONAL Favor de utilizar letra de molde Carrera: Semestre: Promedio: Fotografia Nombre completo: Ap.
Solicitud de Intercambio Academico por Convenio Bilateral UPAEP para alumnos extranjeros INFORMACION PERSONAL Favor de utilizar letra de molde Carrera: Semestre: Promedio: Fotografia Nombre completo: Ap.
Karina Ocaña Izquierdo
 Estudié Ingeniería en Sistemas Computacionales (1997) y una Maestría en Ingeniería de Cómputo con especialidad en Sistemas Digitales (2000), ambas en el Instituto Politécnico Nacional (México). En el 2003,
Estudié Ingeniería en Sistemas Computacionales (1997) y una Maestría en Ingeniería de Cómputo con especialidad en Sistemas Digitales (2000), ambas en el Instituto Politécnico Nacional (México). En el 2003,
Guide to Health Insurance Part II: How to access your benefits and services.
 Guide to Health Insurance Part II: How to access your benefits and services. 1. I applied for health insurance, now what? Medi-Cal Applicants If you applied for Medi-Cal it will take up to 45 days to find
Guide to Health Insurance Part II: How to access your benefits and services. 1. I applied for health insurance, now what? Medi-Cal Applicants If you applied for Medi-Cal it will take up to 45 days to find
EL IMPACTO DEL DOLOR: DATOS EUROPEOS Y ESPAÑOLES
 EL IMPACTO DEL DOLOR: DATOS EUROPEOS Y ESPAÑOLES César Margarit Unidad del Dolor Hospital General de Alicante Member of the Change Pain International Advisory Board PARA PRODUCIR UN CAMBIO NATIONAL HEALTH
EL IMPACTO DEL DOLOR: DATOS EUROPEOS Y ESPAÑOLES César Margarit Unidad del Dolor Hospital General de Alicante Member of the Change Pain International Advisory Board PARA PRODUCIR UN CAMBIO NATIONAL HEALTH
IT Power Camp 3: Project Management with Microsoft Project and PMI
 IT Power Camp 3: Project Management with Microsoft Project and PMI Compuesto por: 1 Jornada Comercial: How to Sell Project Management Solutions with Microsoft and PMI Fecha: 10 de Junio, 2014 Duración:
IT Power Camp 3: Project Management with Microsoft Project and PMI Compuesto por: 1 Jornada Comercial: How to Sell Project Management Solutions with Microsoft and PMI Fecha: 10 de Junio, 2014 Duración:
LAC-2009-09 Modificación 2.3.3.3. DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES DIRECTAS A ISPs
 LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES DIRECTAS A ISPs Current Policy Política Actual 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this
LAC-2009-09 Modificación 2.3.3.3 DIRECT ALLOCATIONS TO ISPs DISTRIBUCIONES DIRECTAS A ISPs Current Policy Política Actual 2.3.3.3. Direct Allocations to Internet Service Providers LACNIC may grant this
SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México
 SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México How did started the Safety Road Show? Airbus Helicopters and others manufacturers did invest since a long time in improving Aviation Safety. In
SAFETY ROAD SHOW 2015 Paul Teboul Co Chairman HST México How did started the Safety Road Show? Airbus Helicopters and others manufacturers did invest since a long time in improving Aviation Safety. In
BOOK OF ABSTRACTS LIBRO DE RESÚMENES
 BOOK OF ABSTRACTS LIBRO DE RESÚMENES 19 th International Congress on Project Management and Engineering XIX Congreso Internacional de Dirección e Ingeniería de Proyectos AEIPRO (Asociación Española de
BOOK OF ABSTRACTS LIBRO DE RESÚMENES 19 th International Congress on Project Management and Engineering XIX Congreso Internacional de Dirección e Ingeniería de Proyectos AEIPRO (Asociación Española de
Chapter Six. Sanitary and Phytosanitary Measures
 Chapter Six Sanitary and Phytosanitary Measures Objectives The objectives of this Chapter are to protect human, animal, or plant life or health in the Parties territories, enhance the Parties implementation
Chapter Six Sanitary and Phytosanitary Measures Objectives The objectives of this Chapter are to protect human, animal, or plant life or health in the Parties territories, enhance the Parties implementation
Kuapay, Inc. Seminario Internacional Modernización de los medios de pago en Chile
 Kuapay, Inc. Seminario Internacional Modernización de los medios de pago en Chile Our value proposition Kuapay s motto and mission Convert electronic transactions into a commodity Easy Cheap!!! Accessible
Kuapay, Inc. Seminario Internacional Modernización de los medios de pago en Chile Our value proposition Kuapay s motto and mission Convert electronic transactions into a commodity Easy Cheap!!! Accessible
CUESTIONARIO Encuesta de prevalencia de autismo. Instituto de Estadísticas de Puerto Rico
 CUESTIONARIO Encuesta de prevalencia de autismo 17 de diciembre de 2010 Cuestionario Trasfondo Este documento contiene el cuestionario de la nueva Encuesta de prevalencia de autismo y trastorno del espectro
CUESTIONARIO Encuesta de prevalencia de autismo 17 de diciembre de 2010 Cuestionario Trasfondo Este documento contiene el cuestionario de la nueva Encuesta de prevalencia de autismo y trastorno del espectro
GENERAL INFORMATION Project Description
 RESULTADOS! GENERAL INFORMATION Project Description The campaign "Adopt a car " had as its main objective to position Autoplaza, the main automotive selling point of Chile, as a new car sales location
RESULTADOS! GENERAL INFORMATION Project Description The campaign "Adopt a car " had as its main objective to position Autoplaza, the main automotive selling point of Chile, as a new car sales location
ERP s Universitarios: soluciones, experiencias y tendencias. CrueTIC Universidad de La Rioja
 ERP s Universitarios: soluciones, experiencias y tendencias CrueTIC Universidad de La Rioja Qué es un ERP? Sistema de planificación de recursos empresariales (ERP, Enterprise Resource Planning). Permiten
ERP s Universitarios: soluciones, experiencias y tendencias CrueTIC Universidad de La Rioja Qué es un ERP? Sistema de planificación de recursos empresariales (ERP, Enterprise Resource Planning). Permiten
Learning Masters. Early: Force and Motion
 Learning Masters Early: Force and Motion WhatILearned What important things did you learn in this theme? I learned that I learned that I learned that 22 Force and Motion Learning Masters How I Learned
Learning Masters Early: Force and Motion WhatILearned What important things did you learn in this theme? I learned that I learned that I learned that 22 Force and Motion Learning Masters How I Learned
CETaqua, a model of collaborative R&D, an example of corporate innovation evolution
 CETaqua, a model of collaborative R&D, an example of corporate innovation evolution CETaqua: manage projects, create value Tomas Michel General Manager, CETaqua September 2011 1. AGBAR: R&D indicators
CETaqua, a model of collaborative R&D, an example of corporate innovation evolution CETaqua: manage projects, create value Tomas Michel General Manager, CETaqua September 2011 1. AGBAR: R&D indicators
Improving Rates of Colorectal Cancer Screening Among Never Screened Individuals
 Improving Rates of Colorectal Cancer Screening Among Never Screened Individuals Northwestern University, Feinberg School of Medicine Contents Patient Letter Included with Mailed FIT... 3 Automated Phone
Improving Rates of Colorectal Cancer Screening Among Never Screened Individuals Northwestern University, Feinberg School of Medicine Contents Patient Letter Included with Mailed FIT... 3 Automated Phone
Prevención Cuaternaria. Cribado de cáncer de mama Uruguay
 Prevención Cuaternaria Cribado de cáncer de mama Uruguay 1 2 3 OPORTUNIDAD O AMENAZA? 4 Ley carne de salud Control periódico toda/os los trabajadores. En mujeres se exige realización de: PAP Mamografía
Prevención Cuaternaria Cribado de cáncer de mama Uruguay 1 2 3 OPORTUNIDAD O AMENAZA? 4 Ley carne de salud Control periódico toda/os los trabajadores. En mujeres se exige realización de: PAP Mamografía
TRATAMIENTO DE ENDOFUGA TIPO II TARDIA
 TRATAMIENTO DE ENDOFUGA TIPO II TARDIA Amer Zanabili, Javier Barreiro, Alejandro Moro, Maria Teresa Pintos, Ignacio Maria Lojo. Servicio de Angiología, Cirugía Vascular y Endovascular. USP - Hospital Santa
TRATAMIENTO DE ENDOFUGA TIPO II TARDIA Amer Zanabili, Javier Barreiro, Alejandro Moro, Maria Teresa Pintos, Ignacio Maria Lojo. Servicio de Angiología, Cirugía Vascular y Endovascular. USP - Hospital Santa
An explanation by Sr. Jordan
 & An explanation by Sr. Jdan direct object pronouns We usually use Direct Object Pronouns to substitute f it them in a sentence when the it them follows the verb. Because of gender, him and her could also
& An explanation by Sr. Jdan direct object pronouns We usually use Direct Object Pronouns to substitute f it them in a sentence when the it them follows the verb. Because of gender, him and her could also
UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda
 UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda EVALUACIÓN IN VITRO DE LA FILTRACIÓN APICAL EN RAICES DE DIENTES EXTRAIDOS, UTILIZANDO DOS MÉTODOS DE OBTURACION:
UNIVERSIDAD DE GUAYAQUIL FACULTAD DE ODONTOLOGÍA ESCUELA DE POSTGRADO Dr. José Apolo Pineda EVALUACIÓN IN VITRO DE LA FILTRACIÓN APICAL EN RAICES DE DIENTES EXTRAIDOS, UTILIZANDO DOS MÉTODOS DE OBTURACION:
PROGRAMA. Operaciones de Banca y Bolsa SYLLABUS BANKING AND STOCK MARKET OPERATIONS
 PROGRAMA 4º Curso. Grado en Administración y Dirección SYLLABUS BANKING AND STOCK MARKET OPERATIONS 4 rd year. Pág. 1 / 8 Colegio Universitario de Estudios Financieros Leonardo Prieto Castro, 2 Tel. +34
PROGRAMA 4º Curso. Grado en Administración y Dirección SYLLABUS BANKING AND STOCK MARKET OPERATIONS 4 rd year. Pág. 1 / 8 Colegio Universitario de Estudios Financieros Leonardo Prieto Castro, 2 Tel. +34
Options for Year 11 pupils
 Options for Year 11 pupils from September and beyond James Slocombe Director of Studies Tom Parkinson Head of Secondary Today sobjectives Explain what choices your son/daughter has and how those choices
Options for Year 11 pupils from September and beyond James Slocombe Director of Studies Tom Parkinson Head of Secondary Today sobjectives Explain what choices your son/daughter has and how those choices
SH 68 Project. Fact Sheet
 SH 68 Project Fact Sheet Why SH 68 Is Needed SH 68 is a proposed 22 mile new road that will connect I-2/US 83 to I-69C/US 281. The proposed new road will connect with I-2/US 83 between Alamo and Donna
SH 68 Project Fact Sheet Why SH 68 Is Needed SH 68 is a proposed 22 mile new road that will connect I-2/US 83 to I-69C/US 281. The proposed new road will connect with I-2/US 83 between Alamo and Donna
Tesis de Maestría titulada
 Tesis de Maestría titulada EL ANALISIS DE CONFIABILIDAD COMO HERRAMIENTA PARA OPTIMIZAR LA GESTIÓN DEL MANTENIMIENTO DE LOS EQUIPOS DE LA LÍNEA DE FLOTACIÓN EN UN CENTRO MINERO RESUMEN En la presente investigación
Tesis de Maestría titulada EL ANALISIS DE CONFIABILIDAD COMO HERRAMIENTA PARA OPTIMIZAR LA GESTIÓN DEL MANTENIMIENTO DE LOS EQUIPOS DE LA LÍNEA DE FLOTACIÓN EN UN CENTRO MINERO RESUMEN En la presente investigación
DEDICATORIA. A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día.
 DEDICATORIA A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día. A mi hermano, que me motiva a seguir siempre adelante. A mi esposo, por estar a mi lado y brindarme
DEDICATORIA A mis queridos padres, por sus enseñanzas y lucha constante para ser lo que hoy soy en día. A mi hermano, que me motiva a seguir siempre adelante. A mi esposo, por estar a mi lado y brindarme
Sistema basado en firma digital para enviar datos por Internet de forma segura mediante un navegador.
 Sistema basado en firma digital para enviar datos por Internet de forma segura mediante un navegador. Autor: David de la Fuente González Directores: Rafael Palacios, Javier Jarauta. Este proyecto consiste
Sistema basado en firma digital para enviar datos por Internet de forma segura mediante un navegador. Autor: David de la Fuente González Directores: Rafael Palacios, Javier Jarauta. Este proyecto consiste
Diseño ergonómico o diseño centrado en el usuario?
 Diseño ergonómico o diseño centrado en el usuario? Mercado Colin, Lucila Maestra en Diseño Industrial Posgrado en Diseño Industrial, UNAM lucila_mercadocolin@yahoo.com.mx RESUMEN En los últimos años el
Diseño ergonómico o diseño centrado en el usuario? Mercado Colin, Lucila Maestra en Diseño Industrial Posgrado en Diseño Industrial, UNAM lucila_mercadocolin@yahoo.com.mx RESUMEN En los últimos años el
Controlling errors in unidosis carts
 1 Control de errores en unidosis Controlling errors in unidosis carts Autor: Inmaculada Díaz Fernández, Clara Fernández-Shaw Toda, David García Marco. Resumen: Objetivo: Identificar los errores en el sistema
1 Control de errores en unidosis Controlling errors in unidosis carts Autor: Inmaculada Díaz Fernández, Clara Fernández-Shaw Toda, David García Marco. Resumen: Objetivo: Identificar los errores en el sistema
